News Blog
Latest News From Our Volunteers in Nepal
VOLUNTEER COMMUNITY CARE CLINICS IN NEPAL
Nepal remains one of the poorest countries in the world and has been plagued with political unrest and military conflict for the past decade. In 2015, a pair of major earthquakes devastated this small and fragile country.
Since 2008, the Acupuncture Relief Project has provided over 300,000 treatments to patients living in rural villages outside of Kathmandu Nepal. Our efforts include the treatment of patients living without access to modern medical care as well as people suffering from extreme poverty, substance abuse and social disfranchisement.
Common conditions include musculoskeletal pain, digestive pain, hypertension, diabetes, stroke rehabilitation, uterine prolapse, asthma, and recovery from tuberculosis treatment, typhoid fever, and surgery.
FEATURED CASE STUDIES
Rheumatoid Arthritis +

35-year-old female presents with multiple bilateral joint pain beginning 18 months previously and had received a diagnosis of…
Autism Spectrum Disorder +

20-year-old male patient presents with decreased mental capacity, which his mother states has been present since birth. He…
Spinal Trauma Sequelae with Osteoarthritis of Right Knee +
60-year-old female presents with spinal trauma sequela consisting of constant mid- to high grade pain and restricted flexion…
Chronic Vomiting +

80-year-old male presents with vomiting 20 minutes after each meal for 2 years. At the time of initial…
COMPASSION CONNECT : DOCUMENTARY SERIES

Episode 1
Rural Primary Care
In the aftermath of the 2015 Gorkha Earthquake, this episode explores the challenges of providing basic medical access for people living in rural areas.

Episode 2
Integrated Medicine
Acupuncture Relief Project tackles complicated medical cases through accurate assessment and the cooperation of both governmental and non-governmental agencies.

Episode 3
Working With The Government
Cooperation with the local government yields a unique opportunities to establish a new integrated medicine outpost in Bajra Barahi, Makawanpur, Nepal.

Episode 4
Case Management
Complicated medical cases require extraordinary effort. This episode follows 4-year-old Sushmita in her battle with tuberculosis.

Episode 5
Sober Recovery
Drug and alcohol abuse is a constant issue in both rural and urban areas of Nepal. Local customs and few treatment facilities prove difficult obstacles.

Episode 6
The Interpreters
Interpreters help make a critical connection between patients and practitioners. This episode explores the people that make our medicine possible and what it takes to do the job.

Episode 7
Future Doctors of Nepal
This episode looks at the people and the process of creating a new generation of Nepali rural health providers.

Compassion Connects
2012 Pilot Episode
In this 2011, documentary, Film-maker Tristan Stoch successfully illustrates many of the complexities of providing primary medical care in a third world environment.
From Our Blog
- Details
- By Lauren Pegoli

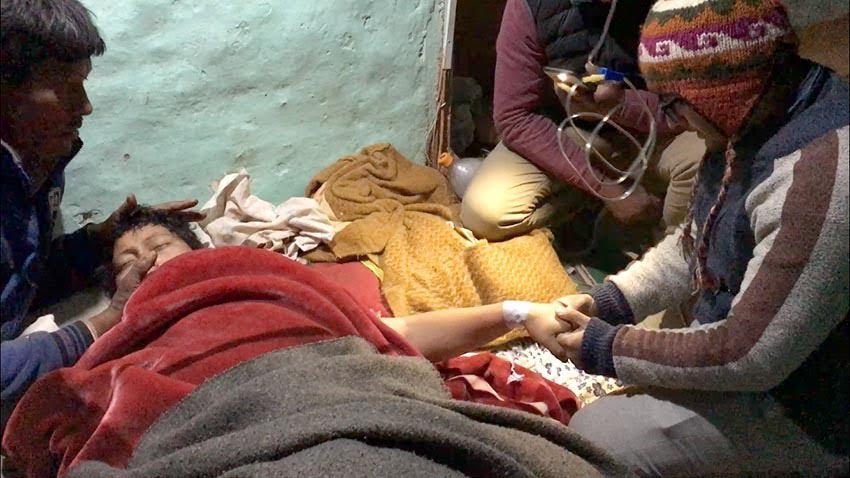
Basanti is a 32 year old woman from the small village of Bajrabarahi, about three to four hours from Kathmandu (depending on your mode of transport). Ten years ago she fell in love with Dikpal; they married and had a child together. She presented at the clinic with stage four breast and brain cancer that had metastasized, possibly spreading to her bones.

Basanti was carried into the clinic by her husband in the early morning. Requesting a bucket be placed beside her bed, within minutes she was throwing up. It was Basanti's first visit to the clinic, her chief complaint being nausea and a one-sided temporal headache. For the past fifteen days she had been vomiting intermittently due to the severity of her pain. The constant sharpness in her left temple was so severe she had been bed ridden for weeks, struggling to keep food and water down. Basanti was initially hesitant to disclose her recent history, possibly because she was weary of further medical intervention. After some time she revealed she had had a mastectomy on her right breast eight months prior, followed by six courses of chemotherapy and twenty-five days of radiation therapy. Almost as an afterthought, she told me of a lump on the left breast that had been itchy for the past few months.
- Details
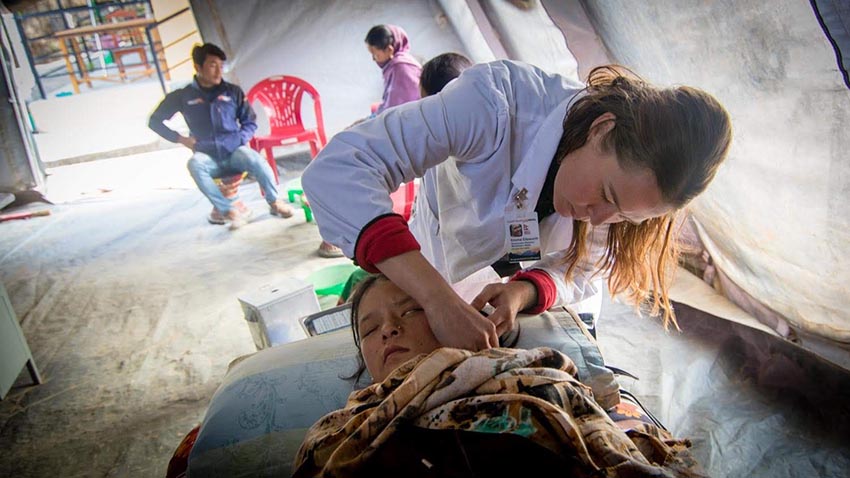
- By Emma Ellsworth

In my first week with Acupuncture Relief Project, a grandmother came to the clinic complaining of abdominal pain. She had eaten some bad buffalo meat and was now suffering from diarrhea and cramping. Despite her discomfort, she had a face that seemed made for smiling. As we discussed her pain, her face broke into a huge goofy grin, perhaps made goofier by the mere four teeth that comprised it. Her eyes twinkled and searched my face as she spoke. I took her vitals, felt her abdomen, gave her advice and treatment. The next time I saw her, she said her diarrhea had ceased and she had returned with a new complaint. As I evaluated her for this new pain, she looked at me and smiled her big goofy smile. She said “You really Love me. You Love me like my mother Loves me.” I was a little bit blown a way and admittedly, tears came to my eyes. My first thought: has no one loved you since your mother? Surely if someone had, you would have referenced that Love, being that you are so far in time from your mother’s Love. My second thought was no, “Love” is too strong a word; I “care” for you as any good practitioner would.

- Details
- By Andrew Schlabach

“Easy! Easy!” My motorbike’s rear tire spins out to the left as it loses traction on the rain soaked, stony... road? path?. It’s a cold wet Saturday morning and I’m wondering how good of an idea it was to come this way. Saturday is usually our day off, but today we are on a mission: three motorbikes slowly winding up through the misty hills near our clinic in Tistung. Mercifully the precarious drop-offs are obscured by low clouds meandering their way through the eerie landscape, giving us the illusion of navigating a precipice surrounded by an endless abyss.
The river is a lot deeper than I expected, soaking my boots. Now climbing the steep muddy bank, I grab a little too much throttle, finding myself slipping somewhat sideways with my bike bouncing ungracefully over the loose stones attempting to gain purchase.
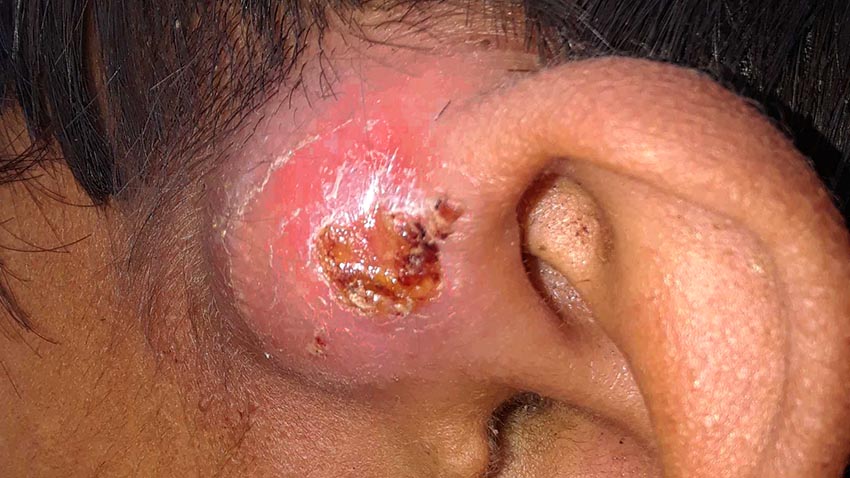
Yesterday at our clinic, a volunteer practitioner, Emma Ellsworth and I managed a rather gory draining of a large skin abscess (carbuncle) on a thirteen year old boy. It was about a one inch, very painful lesion located between his left temple and the root of the ear. The procedure seemed easy enough as we numbed the area with lidocaine, sterilized his skin with povidone-iodine and prepared our tools. After making a small incision using a three-edged needle, copious amounts of turbid yellow puss were drained from the skin. (That was the easy part.) Then, using a sterile stick swab soaked in an antibiotic solution, I inserted the swab several centimeters into the pocket to clean its margins. Thankfully my assistant held steady as we worked quickly to finish the procedure. We dressed the wound, gave our brave young patient some medication for pain and infection, and sent him on his way.
Today we are following up with a house call.
Our Mission
Acupuncture Relief Project, Inc. is a volunteer-based, 501(c)3 non-profit organization (Tax ID: 26-3335265). Our mission is to provide free medical support to those affected by poverty, conflict or disaster while offering an educationally meaningful experience to influence the professional development and personal growth of compassionate medical practitioners.
