Terry Atchley EAMP LAc MAcOM
November 2013
OVERVIEW
 80-year-old male presents with vomiting 20 minutes after each meal for 2 years. At the time of initial visit, patient was vomiting undigested food and water several times per day. Other symptoms include burning esophageal pain, the feeling of constant hunger, and a sensation of “something stopping the food in his chest.” Gastroesophageal Reflux Disease (GERD) and hiatal hernia are suspected causes of vomiting. Vomiting decreased after acupuncture treatments, herbal medicine, dietary changes and the addition of antacid therapy.
80-year-old male presents with vomiting 20 minutes after each meal for 2 years. At the time of initial visit, patient was vomiting undigested food and water several times per day. Other symptoms include burning esophageal pain, the feeling of constant hunger, and a sensation of “something stopping the food in his chest.” Gastroesophageal Reflux Disease (GERD) and hiatal hernia are suspected causes of vomiting. Vomiting decreased after acupuncture treatments, herbal medicine, dietary changes and the addition of antacid therapy.
Subjective
80-year-old male patient reports vomiting 15-20 minutes after meals, burning esophageal pain and a sensation that "something is stopping the food" in his chest. He describes a feeling of fullness after eating, followed by nausea and vomiting. The vomit is watery and contains undigested food. Otherwise, no bloating or discomfort is associated with eating. The pain is a slow, achy sensation and better without food. There is a foul taste in his mouth before eating food, but he is unable to further describe the taste. The patient feels cold most of the time, with only minimal sweating with intense labor, and denies night and spontaneous sweating. Bowel movements are dry and difficult to pass, occurring every 2 days. Nocturia occurs 4 to 5 times per night causing the patient to wake frequently with difficulty falling back asleep. This often leaves him feeling weak and fatigued.
His secondary complaint is wheezing and shortness of breath. He reports a 1 year history of cough with easy-to-expectorate thick, white phlegm throughout the day and night. It is difficult for the patient to take a deep breath, and the wheezing becomes severe when walking. He describes a low-pitched gurgling in his throat during these episodes.
Objective
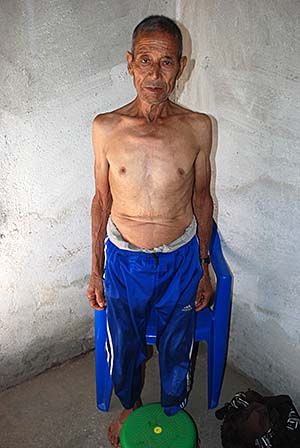
 Patient appears gaunt and emaciated. Each rib is clearly visible, his cheeks are sunken, and his hips protrude. Due to a lack of muscle mass, the skin appears to be draped over the bone. The patient weighs 44 kg and is 162 cm. Body Mass Index (BMI) is 16.8, classifying him as underweight. Upon moderate depth palpation of his abdomen, he feels pain half way between the xyphoid process and the umbilicus along the midline, although no mass is palpable. His teeth have worn down enamel, but the gums are not swollen nor red. On auscultation of the lungs, crackling can be heard in the lower lobes and wheezing in the upper lobes with a respiration rate of 26 breaths per minute (normal range: 16-24). Pulse oximetry shows saturation of 92 percent (normal range 95). (NEED BP AND PR)
Patient appears gaunt and emaciated. Each rib is clearly visible, his cheeks are sunken, and his hips protrude. Due to a lack of muscle mass, the skin appears to be draped over the bone. The patient weighs 44 kg and is 162 cm. Body Mass Index (BMI) is 16.8, classifying him as underweight. Upon moderate depth palpation of his abdomen, he feels pain half way between the xyphoid process and the umbilicus along the midline, although no mass is palpable. His teeth have worn down enamel, but the gums are not swollen nor red. On auscultation of the lungs, crackling can be heard in the lower lobes and wheezing in the upper lobes with a respiration rate of 26 breaths per minute (normal range: 16-24). Pulse oximetry shows saturation of 92 percent (normal range 95). (NEED BP AND PR)
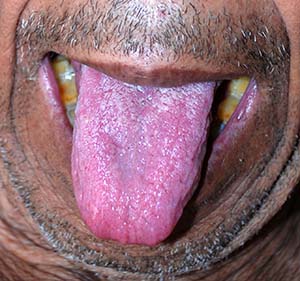
His tongue is dusky in color, tender in texture, with a thick, white coat in the center and back. The pulse is thin and soft.
Assessment:
DX: Gastroesophogeal Reflux Disease (GERD), hiatal hernia or a peptic ulcer could be the cause of the vomiting.
The clinical presentation of GERD is heartburn, with or without regurgitation of gastric contents. GERD is a condition associated with the esophageal sphincter, as is a hiatal hernia. The hiatus is the opening in the diaphragm connecting the esophagus and stomach. A hiatal hernia occurs when the top section of the stomach slides up above the hiatus, pressing against the esophagus. The patient presents with burning esophageal pain and regurgitation of stomach contents, which could be a sign of GERD or a hernia.
Peptic ulcers also present the same as GERD and they are difficult to differentiate without proper imaging. Because this patient’s pain is worse with food it must be considered and empiric treatment is not successful a referral for an endoscopy is required.
TCM DX: Spleen and Stomach Qi Xu with Cold Invasion, Lung Cold Phlegm Accumulation, Kidney Qi Xu
The patient experiences spleen and stomach qi xu through epigastric discomfort, emaciation, distention after eating with a sensation of stuffiness in the chest, fatigue, and nausea. The vomiting occurs when food is eaten, therefore it is an external cold and not internal.
Lung cold phlegm presents with a cough with white phlegm, vomiting of watery fluids, and cold sensations. Given the nocturia of 4-5 times a night, kidney qi xu is also present.
PROGNOSIS: With lifestyle changes such as smaller meals throughout the day to decrease pressure on the weakened sphincter, antacids, herbal medicine and acupuncture, management of the symptoms is expected to have a moderate to significant response. A trial of 10 acupuncture treatments is recommended to assess changes. In the case of a hernia, the resolution is not expected. If significant improvement is not observed by the 10th visit, an endoscopy is recommended with possibility of surgery to repair a hernia.
Initial Plan
Acupuncture: Treat twice per week for 10 visits before reassessing. Focus on tonifying Stomach and Spleen qi, warm excess cold, disperse phlegm accumulation and tonify Kidney qi.
Typical treatment: PC6 (Neiguan), SP4 (Gongsun), CV10 (Xiawan), CV13 (Shangwan), CV6 (Qihai), LU1 (Zhongfu), LU5 (Chize), KI7 (Fuliu), KI3 (Taixi), ST36 (Zusanli); Pole moxa along CV channel of abdomen, ST36, SP4 and LU1
Alternate treatment: BL20 (Pishu), BL21 (Weishu), BL23 (Shenshu), BL24 (Qihaishu), BL25 (Dachangshu), DU4 (Mingmen), KI3 (Taixi); Tiger warmer moxa is used on the back.
Chinese Herbs: Qi Pi Wan, 4g TID, is recommended for 5 weeks to strengthen the Spleen and Stomach. Qi Pi Wan contains the herbs: ren shen, bai zhu, fu ling, lian zi, shan yao, shan zha, chen pi, ze xie and gan cao.
Other treatment: The antacid Digene (magnesium trisilicate and aluminum hydroxide) is recommended to reduce stomach acidity and help with epigastric burning. 1 tablet is to be taken orally before eating meals. A proton pump inhibitor (PPI) is most often the firstline treatment when a patient presents with these symptoms. PPI’s inhibit a mechanism which creates acidity in the stomach. However, a PPI is difficult to obtain in this remote village and Digene is free and available at the local health post. In this case, antacid therapy is prefered as an adjunct to acupuncture and herbal intervention, although a PPI may be reconsidered as the case progresses.
Lifestyle recommendations: Eat smaller meals more often throughout the day; Chew food thoroughly before swallowing; Sleep slightly elevated. Sleeping elevated will help with the GERD symptoms of burning pain by aiding in the descent of food through gravity.
Outcome
After several treatments of acupuncture and adding Digene with meals, the patient reported that the vomiting and burning pain had been resolved. However, the vomiting returned the evening prior to the 5th treatment. Upon further examination, the patient reported he had been eating smaller meals more often, but was going to bed immediately after the last meal of the night. Patient was then counseled on eating meals at least an hour before laying down to reduce the possibility of stagnant food irritating the epigastrium. The patient reported good compliance with his medications and lifestyle recommendations. At the reevaluation (10th visit), the patient stated he could eat a normal-sized meal without vomiting, or sensation of the food stopping in his chest. A reduction in respiratory symptoms was not observed. However, the patient reported an absence of the gurgling sound in his chest during exertion.
Conclusion
The patient is responding well with lifestyle changes, acupuncture, herbs and antacids. Counseling the patient to continue with lifestyle changes could provide the most significant alterations in symptoms. If previous symptoms return, a PPI should be added to the treatment plan. Omeprazole dosed at 20mg PO QD for 4 to 8 weeks and then reassess the patient. If these methods of treatment continue to reduce and eliminate vomiting, future treatment should be focused on reducing respiratory complaints.











