
“Easy! Easy!” My motorbike’s rear tire spins out to the left as it loses traction on the rain soaked, stony... road? path?. It’s a cold wet Saturday morning and I’m wondering how good of an idea it was to come this way. Saturday is usually our day off, but today we are on a mission: three motorbikes slowly winding up through the misty hills near our clinic in Tistung. Mercifully the precarious drop-offs are obscured by low clouds meandering their way through the eerie landscape, giving us the illusion of navigating a precipice surrounded by an endless abyss.
The river is a lot deeper than I expected, soaking my boots. Now climbing the steep muddy bank, I grab a little too much throttle, finding myself slipping somewhat sideways with my bike bouncing ungracefully over the loose stones attempting to gain purchase.
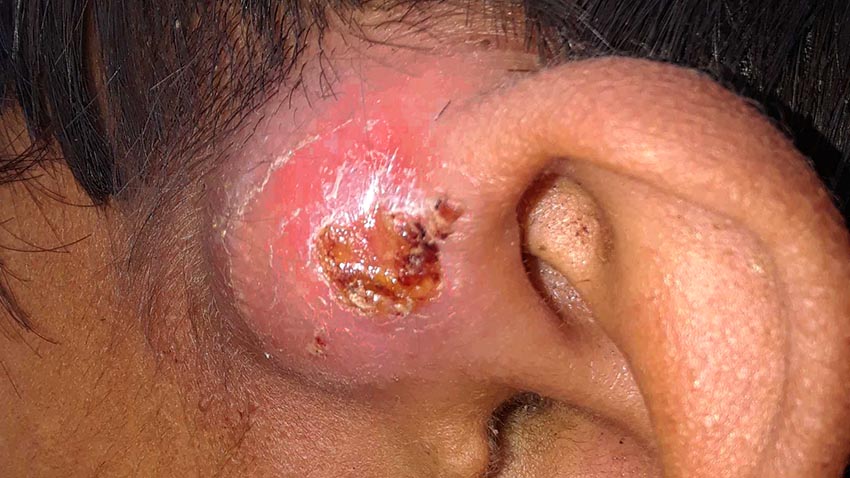
Yesterday at our clinic, a volunteer practitioner, Emma Ellsworth and I managed a rather gory draining of a large skin abscess (carbuncle) on a thirteen year old boy. It was about a one inch, very painful lesion located between his left temple and the root of the ear. The procedure seemed easy enough as we numbed the area with lidocaine, sterilized his skin with povidone-iodine and prepared our tools. After making a small incision using a three-edged needle, copious amounts of turbid yellow puss were drained from the skin. (That was the easy part.) Then, using a sterile stick swab soaked in an antibiotic solution, I inserted the swab several centimeters into the pocket to clean its margins. Thankfully my assistant held steady as we worked quickly to finish the procedure. We dressed the wound, gave our brave young patient some medication for pain and infection, and sent him on his way.
Today we are following up with a house call.

We reach the boy’s home high in the mountains. His family is Tamang, which is an ethnic group in Nepal who’s origin dates back over five centuries. From Mongolian descent, they now maintain their own language and seldom intermarry with other ethnic groups, scratching out a meager existence by growing corn, wheat, potatoes and ganja (marijuana) in the middle hills region across Nepal. Stout, superstitious and all around tough, Tamang people are straightforward to the point of rudeness but love to laugh and are generally hospitable and friendly. Tamang women are adorned with exotic hand-made gold jewelry; usually a large ornate hoop through the center of the nose, or several gold rings in each ear. Facial tattoos are identifying traits on many of the older ladies. I personally find the Tamang people to be both beautiful and intimidating.

As we arrive, several very dirty children peak around the corner of a small dwelling made from the flattened sheet metal of scavenged barrels used to hold pitch for repairing roads. (If you ride the roads of Nepal, you will wonder what that pitch actually got used for. Certainly none of it was wasted on the roads.) We park the motorbikes and start asking for directions. Our party makes its way down a tortuous, slick path between dwellings and fields occasionally diverted by cute baby goats, ponderous water buffalo and unfriendly guard dogs. When arriving at the house, we are welcomed into a simple room piled with bags of ganja, one bed and a simple makeshift table. The room is dimly lit with one small window and the walls are bare stones. We are offered tea, which our frozen fingers gladly accept and we go to work examining the boy’s abscess which is looking pretty good. We clean the site and then considering the boy’s living conditions, decide to give him a stronger antibiotic. We re-dress the wound and ask him to come back to see us when the antibiotics are finished. He and his family agree. Mission accomplished, we make our way back to our motorbikes and begin the slippery decent back to our home in Bajrabarahi.

Since beginning this project over twelve years ago, I have worked to try to understand the needs of the people living in these remote areas and have evolved our project to address those needs. Last year our clinic became the first fully licensed and recognized “Integrated Medicine” clinic in Nepal. But what exactly IS an integrated medicine clinic? That is precisely the question our organization and the Nepal Ministry of Health is trying to answer.

Last year we were able to conduct a large-scale door-to-door census and survey to help set base-line for Non-Communicable Disease (NCD) prevalence in our catchment area. Not only did we capture important data on chronic pain, hypertension, diabetes, breathing disorders, alcohol use, tobacco use and poverty measures for the local and regional government, we managed to do nearly 3000 biometric health checkups in our local community. What we found in doing this was many isolated areas in which our services were not accessible. In these areas we saw so many conditions that simple screenings could have prevented.

This year we adopted a hub and spoke approach to delivering care to more outlying areas. We reduced our staff at our primary clinic in Bajrabarahi and dedicated resources to staffing four satellite clinics in more remote areas. This effort required us to send volunteer practitioners, interpreters and other staff out to these areas by motorbike and tuktuk everyday. A tuktuk is strange looking three-wheeled motorbike with a cabin. I think it would make a pretty awesome ice cream truck back in the United States but, for certain, they are not at all well suited to the roads in Nepal, mercilessly jolting and jostling their passengers over the unforgiving terrain.

Beginning in September, the challenges of this plan became unquestionably apparent. The monsoon rains did not abate until mid October and our teams had to brave flooded roads and landslides. The motorbikes were often bogged down in axil-deep mud, with the rider now struggling to push the bike and the practitioners now on foot. The everyday occurrence of a truck stuck in the middle of the road could cause hour long delays. As the weather cleared in November the roads turned from mud to dust. Teams returning from the field were covered from head to toe in a thick layer of fine powder. And in December, bitter mornings saw teams enduring subfreezing temperatures on their way to our satellites. Our motorbikes, which are built in India, are not really meant for this punishment and require daily health checkups and occasional hospital (workshop) visits. As the Project Director I’m pleased, or rather I should say relieved, to report that since September we have managed to provide over 3500 primary health visits in these outlying areas without any injuries or incidence. (We did lose one iPhone.)

Acupuncture is a wonderful tool in helping rehabilitate patients who have suffered a stroke and we see so many of them in our clinics; too many. Our volunteer practitioners have successfully helped patients walk again, speak again and work again -- which is the power of our medicine. However, I tell our practitioners when they arrive, “I want to stop treating strokes. I want to prevent the next stroke from happening in the first place”. This is a much more difficult challenge. It requires large scale screening of populations, consistent follow-ups of at-risk patients and lifestyle as-well-as medication based management. This concept illustrates what our “integrated medicine” clinic model for rural areas aims to accomplish.
Here are a few of our goals:

First, improve access by going to the patients. The steep and rugged Middle Hills of Nepal present a unique set of challenges. With very few roads, most patients walk for one to two hours over difficult trails to reach larger settlements or roads where they could take a bus to a health facility. It takes about three hours to reach a hospital by ambulance. Elderly populations or people with difficulty walking are especially disadvantaged and often never seek any kind of health services. By using our small fleet of motorbikes or by sending practitioners out on foot, we are able to expand our reach. Volunteers often begin case reports by saying, “My patient is a 62 yo male who has never seen a doctor before in his life. He presents with…”. This is Music to my ears. Fortunately for us, acupuncture affords us a lightweight and cost effective modality for managing many conditions with nothing more than a backpack of supplies. We can assess vital signs, perform basic wellness assessments, look over people's medications, attend to injuries and wounds and basically offer much needed health education and advice -- all of this before doing any acupuncture at all. In cases where we can manage a condition with acupuncture, we set up a treatment plan and set treatment goals. In more complicated cases, we make referrals to our clinic in Bajrabarahi (which is equipped with a comprehensive lab), to a municipal primary care center (the nearest doctor), or to a regional hospital (the nearest specialists). In some cases we help arrange transportation as well.
Second, focus on primary assessment over therapeutics. It is a sunny morning in Bajrabarahi and I am called to the clinic to look at a three-year-old boy. The family has traveled about six hours by bus to our clinic from Hetauda, which is the Capital of Makwanpur (the District in which we operate). Their little boy had suffered a brain injury, technically known as a subacute infarction (basically a type of stroke), a year and a half ago. I could see by the way the boy carried his left hand, curled to his chest and walked with a distinctive limp that this was the case. The parents had heard about our clinic and wanted to see if we could help with acupuncture.

My intern, Sushila Gurung, assisted me with a full examination, interview and review of the boy’s medical records. (Sushila is a wonderfully talented twenty six year old Nepali woman and motivated student. She began working with our project in 2011 as a medical interpreter where she was introduced to acupuncture and our clinical model, later pursuing her own education in the field. Having graduated from her acupuncture school earlier this year, she re-joined our team as an intern student in September and we are very fortunate to have her. Earlier this year, Sushila was accepted for a three-week advanced training course at Zhejiang Chinese Medical University in China Hangzhou. This was her first opportunity to travel beyond her home country and she returned aglow with what she was able to observe and learn during her program in the hospitals there.)

Sushila and I scoured the medical records, looking for clues as to what had happened to the boy. Apparently when the boy was about eighteen months old he developed an inguinal hernia which subsequently developed complications by entrapping and obstructing the bowel. The boy developed a dangerously high fever with convulsions and was taken to a hospital in Kathmandu where he underwent corrective surgery. Unfortunately the damage to the brain had already been done. Since then, the family has been extremely skeptical of hospitals and Western medicine. They have been treating the boy with Ayurvedic herbs which they receive from an Ayurvedic doctor in Hetauda for the last one and a half years. I ask about seizures and the parents describe a history of about five or more seizures a day, sometimes only lasting a few seconds, others lasting over a minute. No sooner do we ask and we see the boy suddenly freeze. His left arm springs out rigidly like he is pointing to something directly to his left and slightly above him. His eyes lock as though he is looking far to the left. Frozen in place just long enough for us to recognize what is happening and then he topples over to the ground, landing stiffly on his right side. He is only a few feet away and by the time we reach him it is over and he happily goes on about his cheerful business apparently ridding our garden of loose stones. I do see that he has several old abrasions on his face and head so I know he had been falling down a lot. Sushila and I set about trying to assess his mental development. He is shy and only speaks a few words. His parents report that vocabulary is limited to about ten to twenty words, which is unusual for a three year old. After about thirty minutes, Sushila and I conclude that the boy is at about fifteen months in his mental development. We also have a look at his gait and use of the left arm. I begin explaining to the parents about our findings and say that I think acupuncture would be helpful but that it would take many visits. They said, “We will do anything! Just tell us what to do!” First off, I explain, we have to manage the seizures and for that I want to get him on some anti-seizure medicine. I explain that these seizures are harmful to his brain development and that we need them to stop. “We know a pediatric neurologist in Kathmandu and we would like to send you there today. Then after you receive the medications we would like you to explore renting a room in Bajrabarahi so that we can see the boy everyday for a month. During this time we can observe him to be sure the seizures are becoming controlled and begin acupuncture and physical therapies.” I also explained that in one month, our therapies will not be curative but will indicate what kind of success we might expect. Our first priority is to eliminate or significantly reduce the seizures. The parents agree, we arm them with a referral letter to the doctor in Kathmandu and they set off for Kathmandu. Sushila and I spend the remainder of the morning charting and discussing the case. I explained to her that I was less concerned about the boys use of his left hand. This was the parent’s primary concern because this was the part they could see but I was much more concerned with the boy’s mental development. “He can live a fully productive life without the use of his left arm but if he cannot learn to speak or read he will be forever limited and this needs to be our primary concern.” I did not point out to the parents that the unmanaged seizures may have been the cause of the developmental delay. I don’t blame them. I blame the Ayurvedic doctor who failed to recognize his therapy was not up to the task. I expect that with proper medication management and consistent acupuncture therapy, this story is going to have an impressive and happy ending.

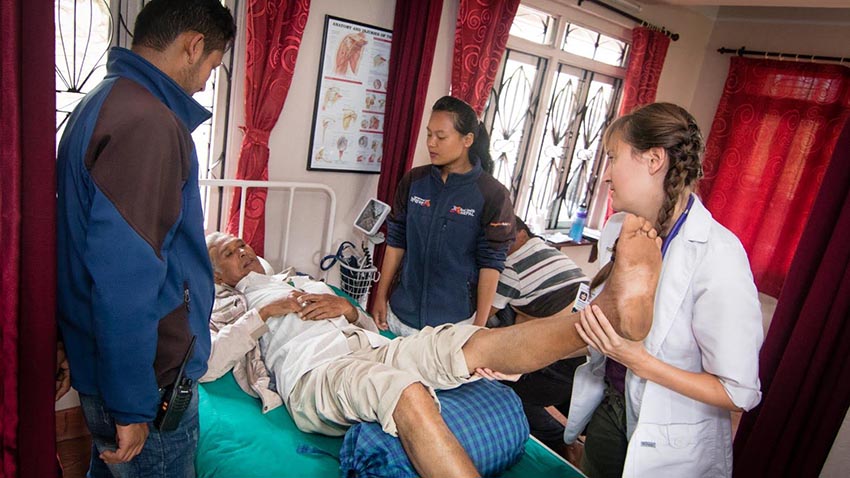
Third, establish strict follow up procedures. In the management of NCDs such as diabetes, primary hypertension or Chronic Obstructive Pulmonary Disease (COPD) and even in some cases of chronic pain, the solution is going to be a combination of consistent monitoring, lifestyle changes, acupuncture (or other manual therapeutics like massage or physical therapy) and medications. One of my team members asked me to have a look at a patient at one of our outreach clinics. She reported to me that the man had a swollen testicle that had been getting worse for two years. She had performed an examination but was unsure of her findings so she asked the patient to return for a follow up. Two days later we met with the patient again. I was already familiar with the patient as he had been receiving treatment from us for a few weeks. He is approximately 70+ (Many elderly Nepali’s don’t know their actual age). He has lived in this village all of his life and he tells us that many of his friends have already died. I can see that he is having a great deal of difficulty breathing and I can hear a gurgling of deep phlegm in his lungs. I examine the testicle which as suspected turns out to be a minor inguinal hernia. At the same time we listen to his lungs, assess his pulse oximetry, take his temperature and reassess his medication. He is already taking the maximum doses of steroidal bronchodilators and is taking supplemental oxygen from an oxygen bottle for thirty minutes, four to five times per day. His daughter-in-law, who has brought him to our clinic, offered a bag of medical records which we review carefully. I explain to both the daughter-in-law, as well as the practitioner, that the man has end stage COPD and that at the moment he seems to be managed. However, between the cold winter nights, his damp unheated house and his poor oxygenation, he is at very high risk of developing pneumonia. He would not be a good surgical candidate to have the hernia repaired and at this point that should not be considered a priority. Our goal should be to help keep him alive through the winter months, which will require close monitoring. We made a follow up plan so that we could track his vital signs and educated the family on several symptoms that could indicate an onset of pneumonia. “If any of these things happen you come to us right away -- don’t wait.” From here we “red flag” the patient’s chart so that we know to call on the patient if he stops coming for follow ups.
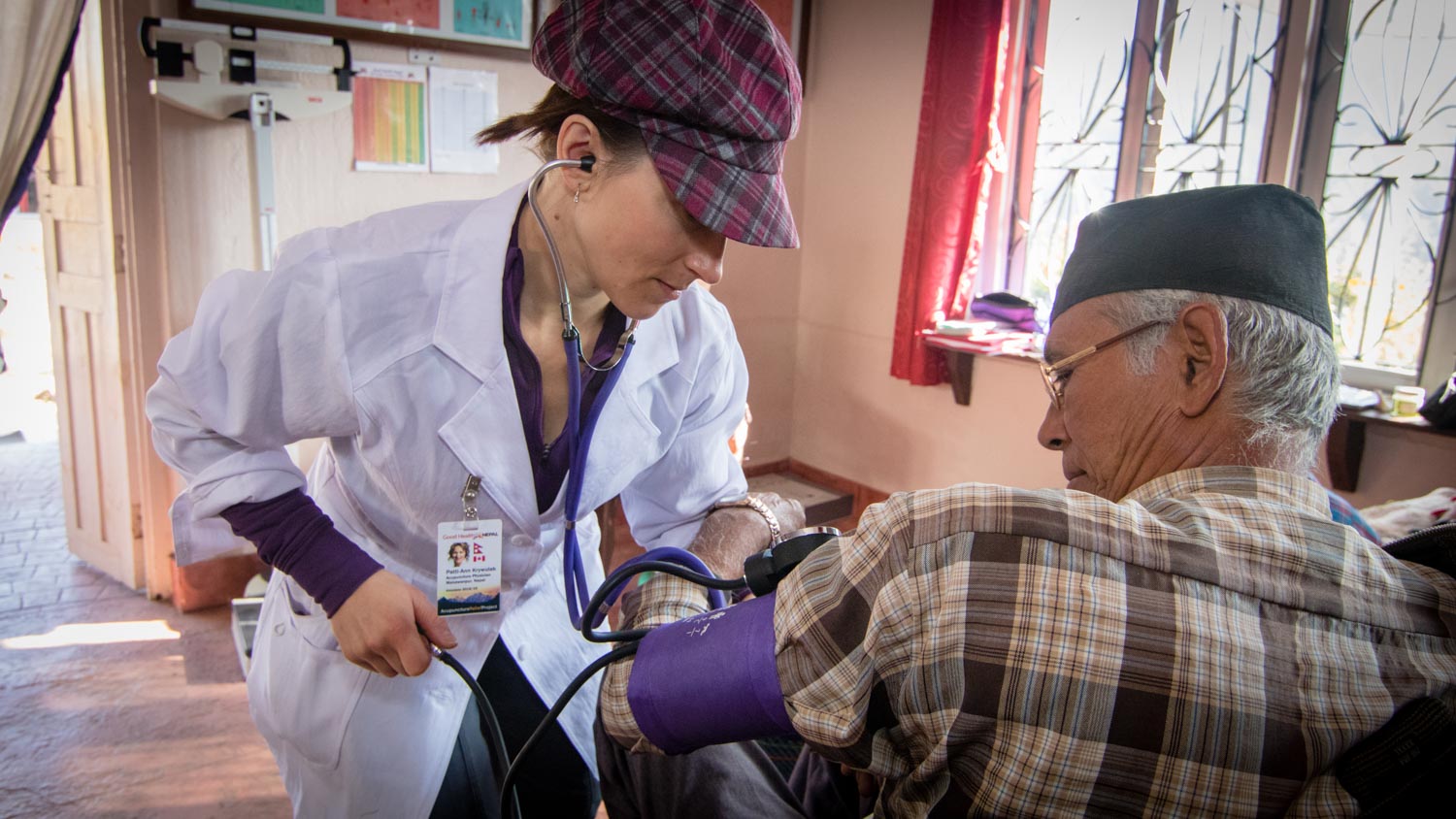
Fourth, establish medication management strategies. My phone rings in the middle of the day and I can hear a trace of anxiety in the practitioners voice as they report that their patient has a blood pressure of 224/128mmHg, a clear emergency. I say, “You know what to do. Providing that their other vital signs are stable and that there are not any other red flags in the case. If the patient cannot be convinced to go to the Primary Health Center (PHC) immediately (which is likely, because there are no more buses running today), go next door to the Health Post and ask the Health Assistant to give three days of emergency Furosemide, 40mg/day. Then make a plan for the patient to go to the PHC within the next five days for assessment and blood pressure medication. Write a referral letter to the doctor at the PHC, reporting the vital signs that we have collected and the medications that have been dispensed. Monitor the patient every day until they are able to go to the PHC and insist that they come back after receiving the medication. Then monitor weekly until management is achieved. Most likely the doctor is going to prescribe 5mg of Amlodipine, which might not be enough, so if we need to adjust the dosage of the medication we can do that remotely with the permission of the prescribing doctor. When the patient is coming in for follow ups, try to figure out why they are having high blood pressure in the first place. I would start by assessing kidney and pulmonary function. You’ve got this! Call me if you need me.”
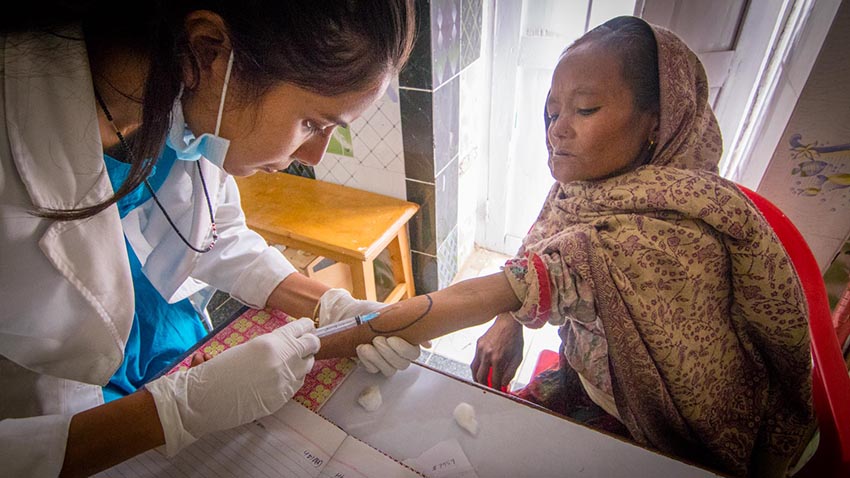
Fifth, provide sustainable, effective and efficient therapeutics. If there is one thing allopathic doctors and acupuncturists can agree upon it is that Western medicine is limited in its ability to manage chronic pain complaints, and that this is one area in which acupuncture really shines. Our research showed the government that pain complaints accounted for about 30% of visits to governmental health facilities and about 20% of government provided medication that people were taking. At our clinic, joint pain (interfering with work) accounted for nearly 70% of our patient load-- obviously a problem that puts a hefty strain on public resources. Fortunately, we were able to show through our research project that almost 60% of our patients claimed that the treatment they received at our clinic was either curative or significantly helpful. This could be implemented at a local level for no more than they are already spending for a Community Health Assistant, would address a broader range of conditions and would be much more effective in the management of NCDs. Through much lobbying of governmental and health agencies, especially at the local, municipal and provincial levels, a couple of unique opportunities emerged.

In Taukhel, one of our satellite clinics, the local government began negotiations with us by offering a clinic building as an incentive to permanently extend our services to their community. Tsering Sherpa, who is my long time friend and project co-creator, also directs our local non-profit (NGO) called Suswathya Nepal (Good Health Nepal). Tsering and I sit in a meeting with the local officials and try to pitch a different idea. We would be interested in taking temporary ownership of the building, refurbishing and establishing it as an adjunctive acupuncture clinic under the authority of the local health post. Our request is that the local community agrees to allocate funds to employ a full-time acupuncturist who we will select and train for the position. After five years we ask that they plan to take the clinic back under their control and budget. Even if this clinic only serves to provide basic wellness assessments and utilizes acupuncture to provide management for both acute and chronic pain, the community will be well served.

In Bhimphedi, a clinic site we maintained for five years from 2013 to 2017, the doctors at the PHC have joined us in requesting that the local government provide an opportunity for an acupuncturist to work within the PHC under their guidance. The two doctors have worked with us in the past -- one as medical student who spent some time observing our clinic operations as part of a rural care outreach program, and another working as a senior doctor at the PHC in Palung, who received our many referral letters and listened to our patient advocacy. They see how useful acupuncture could be in helping with their patient populations, especially in the management of chronic pain and other NCDs. They would like to pilot a program that would result in the first acupuncturist to work at a government health facility in Nepal. The goal would be evaluate and report on this program to the central government, hopefully influencing future policy regarding the management of NCDs. In addition to providing necessary supplies, we have committed to help select, train and provide oversight of an acupuncturist candidate for the duration of the two year pilot.
Whew! There is so much, I could go on for pages. Hopefully I have given you a bit of insight as to the complexity of the work we do here in Nepal. I would like to touch on a couple of brief topics that I just couldn’t figure out how to address in my format, so please bear with me. These are policy ideas that are actively developing and are as of yet mostly just problems without apparent solutions.

Palliative care for the dying: In the coming weeks you are going to be reading a powerful blog from volunteer practitioner, Lauren Pegoli. I won’t ruin it but it involves a young woman who was brought to our clinic suffering from stage four breast cancer. She had already undergone as much treatment as her family could afford and the cancer had spread throughout her body and into her brain. Lauren, Tsering and I discussed our role at length and a plan was made to provide as much relief as was practical during her dying process. Drugs that would commonly used in hospice care, such as morphine, are prohibited in Nepal and even minor opiates like Tramadol (a drug that might be prescribed in the United States for back pain or dental pain) are not accessible at a local level. During my tenure in Nepal, we have been involved with many patients who have passed away-- sometime peacefully and sometimes in agonizing pain or slowly suffocating from breathing difficulties. Now, I am certainly not an expert in this area of medicine but I think we can do better. Fortunately the government of Nepal is thinking about this problem as well and the topic is becoming commonplace in policy meetings, but so far I have seen little action. Often in our catchment area, our volunteers are the only health providers responding to these cases. As the areas become even more remote, no one is responding. Even simple things like educating the family and providing the patient with basic hygiene are sometimes amiss. I hope to participate in the practice and policy development regarding the future of this topic in Nepal.

Education of local providers: I am blessed with many volunteers from all over the globe, who see the potential in our small project and come to participate, struggle and learn. We provide volunteers with over sixty hours of training in rural healthcare and a unique clinical structure, which allows them to improve their diagnostic and case management skills. The new skills they acquire through this immersive experience is taken back to their home countries to serve their own communities. This is one of the areas in which we are truly effective. However, after twelve years we are entering a new phase in our development in which we will attempt to sustain without foreign volunteers. We are still several years from this but here is what we have so far. We have sponsored several students to attend the only acupuncture school in Nepal and several of them graduated just this year. The school only has a vocational training accreditation and I am hoping that one day a Bachelors level program can be established. At this point, students receive one year of basic sciences, one year of theory and a one year clinic practicum. This allows them to receive a license to practice under supervision. From here it takes several years of experience and mentorship to learn the elements that are required to practice within our model. Satyamohan Dangol has been working with me since 2008 and is becoming a very skilled and independent provider. As I mentioned previously, Sushila Gurung joined our team this year and is beginning to see her own patients as well. But if we are to truly self sustain, penetrate the governmental health system and expand our model into other regions, I will need dozens more.
I would like to dedicate this entry to my Board of Directors: including Sheri Barrows and Diane Wintzer, who do endless amounts of work behind the scenes to enable me to run this project. Elissa Chapman who has served as our Clinic Director in Nepal for the past four years and has been a critical part of our establishment in Bajrabarahi. The Board of Directors of Suswasthya Nepal, especially Tsering Sherpa who’s dedication, wisdom and especially patience, has moved mountains. Also, to all of our advisors and team leaders including Sarah Richards, Emma Sanchez, Terry Atchley and Bex Groebner, who generously dedicate their expertise and time to the advancement of our goals. Our wonderful staff of interpreters, receptionists, cooks, cleaners and managers -- we would be lost without you. Anupa Timalsina who runs our “Best Lab in Nepal” and who I wish all the best for her upcoming wedding. And finally, to our generous donors: I hope that this accounting of our project will make you smile with pride. On behalf of everyone involved, I sincerely thank you for believing in this vision and helping make it possible.
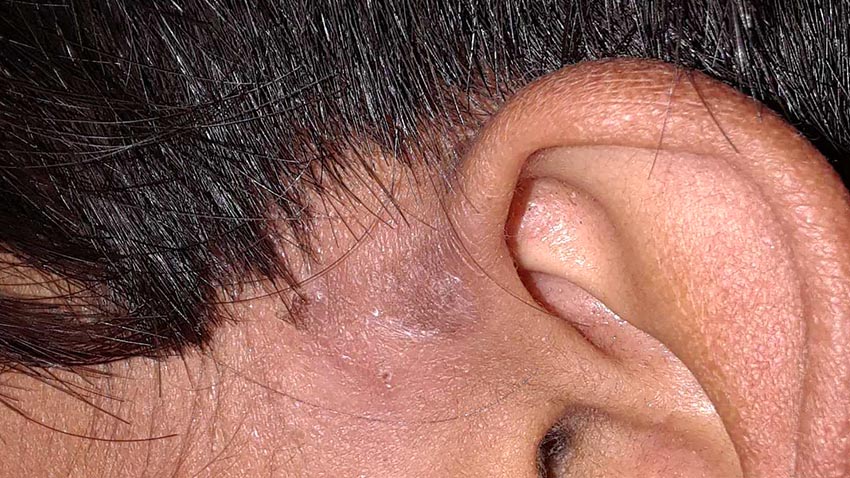
Oh, and if you are wondering about that Tamang boy’s ear -- well, within about ten days he was fully recovered. I expect we will be reading more about that case from the practitioners perspective in the coming weeks.

As I end my year in Nepal and prepare to turn the next camp over to Team Leader, Emma Sanchez, I enjoy one last motorbike ride though the hills of Makwanpur on my way back to Kathmandu. It is December 31st and it is frosty and clear. My fingertips and cheek bones ache from the cold but it is hard to complain. I am treated to a spectacular view of the Himalayas as I clear the top of the pass and look down at the Capital. I marvel at the towering fortress of mountains from Mt Everest to Annapurna and I am filled with gratitude, to be right here in the middle of this experience. --- Andrew
Author: Andrew Schlabach, MAcOM EAMP
Director, Acupuncture Relief Project
Bajrabarahi, Thaha, Makawanpur Nepal












