Kimberly Shotz WHCNP MN MAcOM
December 2011
Overview
 10-year-old female presents with active phase of Juvenile Rheumatoid Arthritis (JRA) as demonstrated by multiple articular bony joint deformities, severely limited range-of-motion in all affected joints, and a history of recurrent episodes of alternating fever, chills and profuse sweating, immediately preceding joint inflammation and swelling. Within the course of 9 acupuncture and moxibustion treatments plus Chinese herbal and vitamin supplementation, the patient noted cessation of recurrent episodes of fever, chills and sweating, decreased heat sensation in joints with active inflammation, and temporary decreases in pain while walking.
10-year-old female presents with active phase of Juvenile Rheumatoid Arthritis (JRA) as demonstrated by multiple articular bony joint deformities, severely limited range-of-motion in all affected joints, and a history of recurrent episodes of alternating fever, chills and profuse sweating, immediately preceding joint inflammation and swelling. Within the course of 9 acupuncture and moxibustion treatments plus Chinese herbal and vitamin supplementation, the patient noted cessation of recurrent episodes of fever, chills and sweating, decreased heat sensation in joints with active inflammation, and temporary decreases in pain while walking.
SUBJECTIVE (as reported by patient’s father)
The patient was evaluated by allopathic medical physicians at a Kathmandu hospital at least 2 years prior to her first visit to VVHC. Blood tests and x-rays (not available for review) indicated rheumatoid arthritis. She was prescribed multiple medications, which she took for 2 weeks. Medications included injections she was advised to receive weekly for 4 weeks. She had 2 injections, which “had no effect.” All medications were too expensive to continue. The patient’s father refuses to involve allopathic medicine in the current management of the patient’s disease, but agreed to update blood tests (CBC, ESR).
Patient presents with hot, swollen ankles and knees, making it too difficult for her to attend school.
O – 6 years ago with 3-4 days of tidal fever, cough and “cold”
F – Fevers come every week to 3-4 months and last about 4 days. They are preceded by a sensation of inflamed tonsils and are followed by joint swelling and a sensation of heat in the affected joints, which are warm to touch, but with or without redness and pain.
Q – Affected joints vary with each episode, but are typically bilateral. Without fever, most joints feel cold and stiff inside.
P – Cold weather and prolonged immobility, such as bus rides, seem to worsen her overall joint stiffness. Swelling increases with mobile activities, such as walking. Wearing warm stockings helps reduce stiffness.
S – Patient reports significant difficulty with ambulation due to both restricted ROM and occasionally severe pain.
T – The duration of active, inflammatory phases is unclear, but seems variable.
Objective
Patient’s affect is flat and timid, with infrequent eye contact. She does not speak and looks to her father for answers to physician questions. She nods occasionally. She ambulates slowly with rigid, erect posture, arms extended and inanimate at side, with somewhat of a shuffle and notably reduced knee and foot flexion.
Her tongue is purple red with a crimson tip and thin white coat at back. She has erythematous sublingual sores (ulcers). Her pulses are thin and rapid.
She displays no observable expressions of pain during palpation of affected joints, but quietly gasps and retracts (i.e. guards) her limbs with attempts to move a joint beyond its passive ROM.
Elbows: Lateral epicondyles are enlarged, rounded (2X normal), bony-hard, cool, without erythema or edema and non-tender; Limited extension to ~145 degrees
Wrists: Mildly enlarged (<2X), bony landmarks obscured to palpation, non-tender; No active or passive extension; Active/passive flexion ~ 20 degrees; Inversion/eversion <10 degrees with mild crepitus of right wrist
Hands/Fingers: Mild bony enlargement of proximal and medial interphalangeal joints bilaterally, cool; Patient unable to flex fingers into fist
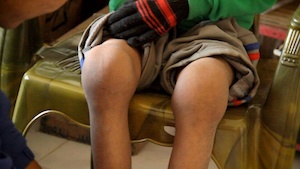
Ankles: Swollen, red, hot
Knees: Soft swelling over medial and lateral femoral and tibial condyles (3X normal)
Active and Passive Range-of-Motion:
Neck: Extension ~0 degrees, flexion ~10-20 degrees, lateral rotation ~10-20 degrees, lateral flexion ~30 degrees to pain
Wrists: Extension ~0 degrees, flexion ~45 degrees, inversion/eversion ~10 degrees
Fingers: DIP/MIP flexion <45 degrees, first and second MCP flexion ~20 degrees
Knees: Extension ~75-80 degrees
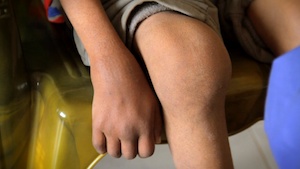
Ankles: Dorsiflexion ~0 degrees, non-painful crepitus near talus with inversion 5-10 degrees of right ankle, eversion ~5 degrees, plantar flexion <45 degrees
Laboratory (2 years ago)
Hemoglobin (HGB): 8 (very low)
White Blood Cell Count (WBC): 14 (elevated)Neutrophils: Elevated
Erythrocyte sedimentation rate (ESR): 30-50 (elevated)
Laboratory (11/24/11)
HGB: 9.5 (low, improved)
Neutrophils: 81 (elevated)
WBC: 11 (mildly elevated, improved)
ESR: 90 (significantly elevated, active phase)
Weight: 22kgOral temperatures (in sequence of visits): 94.4, 97.1, 95.5 (variable, low)
Assessment
DX: Polyarticular arthritis, systemic juvenile arthritis with osteopenia (Still’s disease)
TCM DX: Shaoyang or blood level heat/heat bi syndrome; bony bi/ wind-cold-damp with latent damp-heat toxin
PLAN
Treatment principles: Warm and open the channels and collaterals, move qi and blood, dispel cold, damp, wind, nourish blood, tonify qi, blood and 5 zang organs (constitution). Induce prolonged remission phase of JRA, prevent recurrence of active phase of disease by strengthening constitution and promoting optimal immune function. Treatments consist of combinations of in/out and sustained needle acupuncture, indirect moxibustion and refilling herbal prescriptions and dietary supplements.
Dietary advice: Avoid night shade vegetable family, animal fats, greasy/fried foods, sugar and spicy foods. Increase oral hydration of warm fluids and incorporate cinnamon and turmeric into meals.
Dietary supplements: Calcium 500mg, vitamin D3 500 IU per day, B-complex 1 tab once daily, ibuprofen 20-40mg/kg/day in 3-4 divided doses (not to exceed 880 mg in any 24-hour period) for no more than 5-7 days without clinic evaluation (Liver and renal function labs need to be updated)
Herbs: Feng Shi Ding 2-3 pills BID
Acupuncture: 3 times per week
The following acu-points are used: SP9, LI11, LI10 TB5, GB34, BL11, LR3, LI4, TB3, LI5, SI7; In/out needling: DU14, ST34, SP9, ST36, BAXIE, ST36, KD3
Limit to 8-9 points per treatment.
Auricular acupressure seeds (1 visit): Shenmen, Kidney, Liver, Knee applied bilaterally to leave in place for 3-4 days
Indirect Moxibustion: ST36, elbows, wrists, dorsal hand/MCPs, ankles
OUTCOME
Patient noted reduction in both pain and difficulty with ambulation immediately following treatments. The father reported cessation of alternating fever, chills and profuse sweating episodes as well as an improvement in her energy. The duration of pain reduction benefit was limited to 2-3 days. Patient’s shen appeared brighter and showed increased interest and attentiveness during her treatments. She was able to actively extend her legs to 180 degrees and dorsiflex her ankles to ~5 degrees. The first and second MCP joints had 30 degrees flexion. After treatment 5, ankles no longer felt hot and her knees were warm without erythema.
At her 6th visit, the formula was changed to Xuan Bi Tang Wan 3 tablets TID. A stronger blood/qi/KD nourishing herb was being considered for her 9th visit, given that the joint swelling and inflammation was waning. Liu Wei Di Huang Wan was chosen and dispensed to patient at 9th visit, 8 TID.
Because it took 6 hours of public transportation to get to and from the clinic (>18 hours of missed work per week for patient’s father), this schedule was not feasible. Patient received treatments every 3-7 days for 8 treatments.
Conclusion
This young patient has a severely disabling, progressive disease and lacks resources required for allopathic management regimens known to induce and prolong remission phase and reduce joint destruction associated with Juvenile Rheumatoid Arthritis (JRA).
Each day that severe, active-phase joint inflammation continues, indicates potentially permanent joint damage, reduced mobility and reduced quality of life for patients with JRA. The patient’s father accompanied her to most clinic appointments and provided a limited and inconsistent history of her disease condition, possibly indicating cultural-conceptual and/or practitioner-patient communication challenges. This definitely represented a barrier to optimal assessment of her condition. It was clear from his account of her history that he did not understand the disease process of JRA, its management, or the implications of ineffective management.
The long distance between home and clinic resulted in excessive time away from work for her father, which severely limited treatment frequency and potential efficacy. This patient was unable to maintain the optimal 3-4 times weekly treatment schedule, yet still noted both subjective and objective improvements during the course of her 9 visits over 6 weeks: increased joint range-of-motion, reduced joint inflammation, cessation of systemic inflammatory symptoms, improved constitutional energy and spirit.
It is expected this patient would benefit from incorporating massage and physical therapy into her treatment regimen. Some of her reduced joint mobility seems to be from muscular contraction due to the combination of prolonged guarding of joints and limbs and reduced mobility. A more aggressive treatment plan using a greater number of acupoints with longer needle retention, plum blossom, jing-well acupoint bleeding, scalp acupuncture and/or electroacupuncture may enhance treatment efficacy and may be employed as patient comfort permits.











