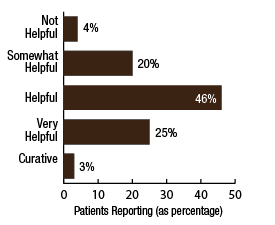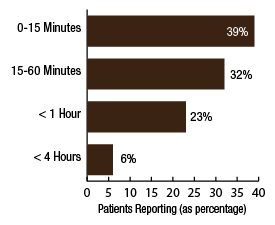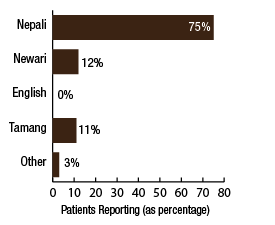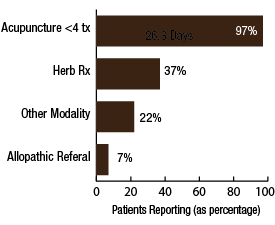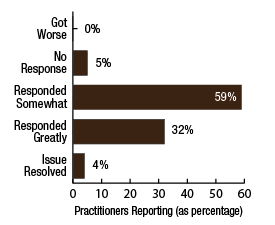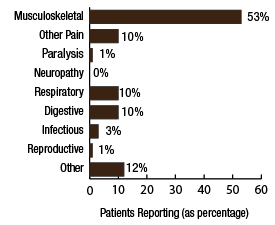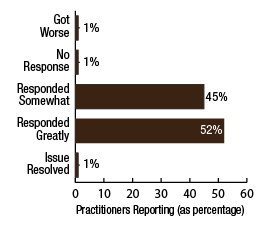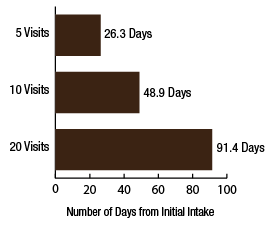Acupuncture as primary care in rural Nepal: a practice-based clinic overview survey studyAndrew Schlabach, Christa Caputa, John Gunnar Ramstedt, Kelli Jo Scott, Andrew VuAbstract: Acupuncture Relief Project (ARP) conducted a practitioner/patient survey of its operations at the Vajra Varahi Health Care Clinic in Chapagaon, Nepal and associated outreach health clinics between September 15, 2011 and March 1, 2012. The survey included the collection of demographic information and provides a clinic-wide overview of patient assessment, prognosis, and treatment outcomes. Background: Acupuncture Relief Project (ARP) operates a primary care health care clinic in rural Nepal which was founded in 2008. Over the past four years, practitioners from ARP have conducted over 100,000 patient visits in the course of providing cost-effective health care and treatment in undeserved and impoverished communities. The goal of this project is to document clinic operations in order to help guide future research in Nepal as well as contribute to a growing body of evidence that uses acupuncture to deliver primary care in developing countries and rural environments. Findings: Demographic and chief complaint data was consistent with care provided in Complementary Alternative Medicine (CAM) clinics as well as allopathic Primary Care clinics in the United States. Clinical outcomes were comparable with those reported by other CAM clinics. Conclusions: The overview survey completed by the Acupuncture Relief Project in Nepal was successfully implemented. Not only was the demographic data gathered to better treat and address the most prevalent concerns of patients, but the implementing of the survey became a teaching tool for practitioners to shed their subjective data gathering and rely more on their objective data-gathering skills.
|
|
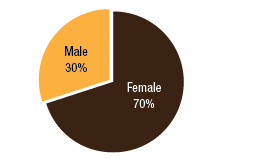
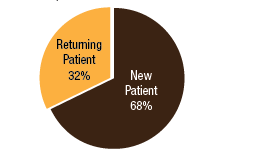
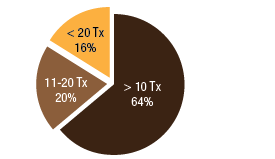
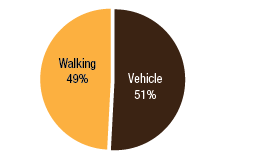
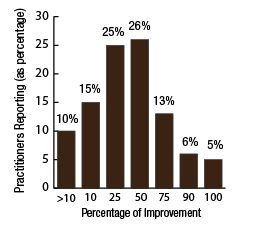
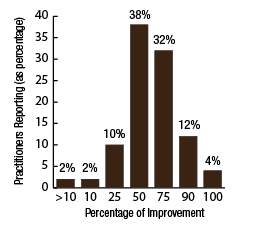
BackgroundNepal remains one of the poorest countries in the world and has been plagued with political unrest and economic instability for the past two decades. Acupuncture Relief Project (ARP) practices in Chapagaon, Nepal and villages in the surrounding area. Over the last four years ARP has provided over 100,000 treatments to patients living in rural villages outside of Kathmandu, Nepal. Their efforts include the treatment of patients living with HIV and AIDS as well as people suffering from extreme poverty and social disfranchisement. Common conditions include musculoskeletal pain, digestive pain, hypertension, diabetes, stroke rehabilitation, uterine prolapse, asthma, and recovery from tuberculosis treatment, typhoid fever, and surgery. ARP conducted a survey in an effort to gain a “big picture” perspective of the clinic operations and assess who and what they are treating in order to guide further research and improve efficacy of treatments. This survey was conducted from September 15, 2011 through March 1, 2012. A Patient Reported Outcome Measure (PROM) enabled the clinic team to use a standard survey to collect their data created particularly for their population. Patient Reported Outcome Measures utilize patients’ perspectives on the progress of their wellness. The clinic researchers had three goals for the survey; to collect demographic data on the patients, to collect data regarding efficacy of treatments, and to create a common platform where practitioners and patients can communicate. Out of 519 patients who answered the language question, only one spoke English and most patients are illiterate in their native language. Because of these specific limitations unique to the population that frequents the ARP clinics, it was determined that an oral survey utilizing a medical language interpreter would be the appropriate tool. Appropriate assessment is also difficult in these clinics. When practitioners volunteer to serve in Nepal, they are operating in a foreign environment. They need an interpreter to communicate with their patients, and the cultural differences can create an enormous disconnect between practitioner and patient. ARP needed a tool to bridge those gaps in communication. Utilizing the survey actually encouraged practitioners to utilize more objective measures in their assessments and provide better prognosis information to their patients. In addition, ARP hoped to show patterns in the length of time in which symptoms began to resolve. There is no other research published regarding the chief complaints most often seen in rural Nepal clinics. Our findings may allow some generalization about the needs of these particular populations. MethodsThe overall purpose of this survey was to determine the types of cases that are being treated at the Acupuncture Relief Project’s clinic in Chapagaon, Nepal, as well as the efficacy of those treatments, and the local community’s perception of the treatments being received. Basic demographic information (age, sex, primary language, and how far the patients traveled to get to the clinic) was also gathered. The questions in this survey were written specifically for this investigation. ARP runs for five months each year. The survey was taken for that duration to give a snapshot of one annual cycle. There were four similarly designed sections to the survey, one to be filled out at each the first, fifth, tenth, and twentieth treatments in the clinic. Their purpose was to rate the progression or decline of the initial chief complaint that brought them into the clinic. For each of the treatments after the first, there was a subjective section to be filled in with the patient’s assessment of their progress and an objective section to be filled out by the clinician based on their observation and assessment of the patient’s progress. A five point scale was used and the answer choices were as follows: has gotten worse despite the treatment, has not responded to the treatment, has responded somewhat to the treatment, has responded greatly to the treatment, and has been resolved. Clinicians were also asked to use a combination of subjective information collected from the patient and their objective observations to assess the percentage that the chief complaint had resolved since the survey initiation. Answer choices were: less than 10%, 10%, 25%, 50%, 75%, 90%, or 100%. The second purpose of this survey was to train volunteers how to better evaluate and assess patient cases and see how it is different in this clinical environment (given language barriers, cultural perceptions, etc.) than it is in a typical Western setting. There were questions specifically designed to direct and teach the clinicians to estimate how long it may take for the patients to get better, or to see a change in the condition of the chief complaint. This part of the survey included two sections; 1) Assessment, with five possible answer choices being: significant improvement expected within five treatments, ten treatments, beyond ten treatments, significant improvement expected with allopathic care, or significant improvement not expected. 2) Plan, with response options being: patient to be treated at this clinic, patient to be treated at this clinic in support of allopathic care, patient to be examined and referred to allopathic care, patient examined but not treated. During the fifth and tenth treatments the patient charts were reviewed to see if any Chinese herbs were prescribed or if any referrals to other practitioners were given. The surveyors were also asked to record any secondary complaints that had arisen for the patients and if there were any, they were also evaluated, as above, at subsequent appointments. The survey was administered orally during the initial intake to the clinic by the practitioners who each received two hours of training to standardize the responses. Periodic reviews of the surveys were done to insure proper documentation. The clinicians were assisted by Nepali interpreters, who are integral to the running of this clinical setting. Each interpreter has received a minimum of forty hours of training in medical concepts and terminology. They each have one to four years of experience working in this clinic. The practitioners were volunteers and all held master’s degrees or the equivalent, depending on their country of origin, in acupuncture and Oriental Medicine. Their experience ranged from recent graduates to five years in clinical practice. Five hundred thirty-four surveys were completed and the data was compiled and input by a research group of master’s students in their final year at Oregon College of Oriental Medicine. The quantifying software used was Fluid Surveys and Microsoft Excel. Fluid Surveys was the primary software used to input data and to gather information. Microsoft Excel was used to calculate the average number of days between the first treatment and their fifth, tenth, and twentieth treatments. Scatter graphs were also made using Excel to give a clear visualization of the data due to the extensive sample size. This survey was funded by Acupuncture Relief Project. Demographic FindingsApproximately 542 surveys were completed during this five month period of time. Seventy percent, (378/542) of respondents were women and 30% (164/542) were men [Table 1]. Patient age was tallied and there was a wide range with all age groups represented. The most common age group was 46-55 years old at 22% (119/528) of those polled. Age 0-16 year olds made up 3% (16/528), 17-25 were 6% (36/528), 26-35 year olds represented 13% (73/528), 36-45 year olds were 19% (36/528), 56-65 year olds 17% (94/528), 66-75, 12% (67/528) and the oldest group, those 76 and older, were also 3% (21/528) [Table 2]. Sixty-eight percent, (354/517) of the patients surveyed were new to this group of practitioners in the clinic and 32% (163/517) had been seen in the clinic at some point in the past [Table 3]. Of those returning, 64% (83/129) were seen less than 10 times, 20% (26/129) 11-20 times and 16% (20/129) were seen more than 20 times [Table 3a]. These final 16% are the more chronic disease cases probably requiring long term frequent care to maintain their current level of health. As a gauge of public opinion, the returning patients were also asked, “Has the treatment at this clinic been helpful?” Responses of those 157 patients polled who had been seen before in the clinic were as follows: the majority, 46%(73) found it helpful, 25% (40) found it very helpful, 20% (32) somewhat helpful, 4% (7) not helpful, and 3% (5) found it curative [Table 4]. In addition to the primary clinic in Chapagaon, there are several outreach clinics in outlying communities. The mountainous terrain of this region and its lack of roads present special transportation challenges for the more severe cases and the most debilitated patients. Traveling to the clinic in such conditions and back again can potentially negate the benefits of the treatment received. In these instances, team members will set up clinics out in the village schools or other public spaces or even on rare occasions, serve patients in their homes, typically traveling with an interpreter thirty to sixty minutes on a motor bike to the more remote areas of the region. Thirty-four percent, (183/536) of the surveyed patients surveyed were seen in these outreach clinics and 66% (353/536) were seen at the primary clinic in Chapagaon [Table 5]. Forty-nine percent, (249/506) of the patients arrived at the clinic on foot and 51% (257/506) used a vehicle, which in almost every case is public transportation [Table 6]. This public transportation includes overcrowded busses and small vans carrying 25+ people. It is not uncommon to see elderly people in need of care, outside on the top of a van or bus, having traveled long distances over rugged terrain to get to the clinic. This survey also included demographics for how long the patients traveled to get to each clinic. Thirty-nine percent, (200/518) took 0-15 minutes, 32%(168/518) took 15-60 minutes, 23% (120/518) took greater than one hour and 6% (30/518) took greater than 4 hours to travel one-way to this clinic [Table 7]. Most patients in Nepal speak more than one language, including in some cases English. But generally, they are most comfortable communicating in their local dialect whenever possible. The survey question was asked to patients as, “What language do you speak best?” [Table 8]. Findings were that out of the 519 responses to this question 75% (387) spoke Nepali, the national language, 12% (60) spoke Newari, the common local language of Chapagaon, 11% (58) used Tamang, a common language in villages outlying Chapagaon. There were 3% (13) who spoke other languages, including Gurung, Magar, Sherpa, Kirati, Tibetan, and 0% (1) spoke English. Clinical FindingsInitial Exam Five Visits Practitioners were trained to use a combination of patient-reported information obtained through their interview and objective measures in the patient chart to assess the patients’ progress. This information was reported in two ways. First, practitioners assessed how much of the overall chief complaint had been resolved [Table 11]. This assessment showed that of 218 respondents, 51% (112) showed 25-50% improvement of their chief complaint, 24% (52) showed greater than 75% improvement, and 25% (54) showed 10% or less response. Second, practitioners assessed how the patient’s response compared with the treatment plan [Table 12]. For example, a stroke patient showing 10% improvement at 5 treatments would indicate a good response whereas a patient with a minor muscular strain showing 10% improvement at 5 treatments would indicate a poor response. This assessment showed that of 218 respondents, 60% (131) showed some response and 30% (66) showed a better than expected response to treatment. Also at the fifth visit, secondary complaints were recorded [Table 13]. Fifty-three percent, (78) of the 146 patients that reported were now concerned with a secondary musculoskeletal complaint. Ten percent, (15) reported other pain pathologies, 10% (14) respiratory complaints, 10% (15) digestive complaint (all of which were diagnosed as chronic gastritis) and 12% (17) had other complaints including hives, insomnia, fatigue and emotional imbalances. Ten Visits Utilizing the same combination of subjective and objective measures as used in the 5th visit assessment, practitioners evaluated patient progress. The majority of patients saw dramatic improvement of their original chief complaint over the course of their treatment [Table 15]. This assessment showed that of 76 respondents, 55% (43) showed 50-75% improvement of their chief complaint, 16% (12) showed greater than 90% improvement and 28% (21) showed 25% or less improvement. Assessment of patient response compared with the expected response recorded in the treatment plan [Table 16] showed that of 77 respondents, 45% (35) showed some response and 52% (40) showed a better than expected response to treatment. Number and Frequency of Patient VisitsAcupuncture Relief Project teams at the Vajra Varahi clinic serve approximately 70-90 patients per day and offer frequent follow-up treatments. During the survey period, 534 new patient visits were surveyed. Of these patients, 42% (226) continued care to fifth visits with the average number of days between initial intake and fifth visit being 26.3 days (treatment every 5.26 days). Fifteen percent, (79) of patients continued care to 10 visits with the average number of days between initial intake and 10th visit being 48.9 days (treatment every 4.89 days). Two percent, (11) of patients continued care to 20 visits with the average number of days between initial intake and 20th visit being 91.4 days (treatment every 4.57 days). DiscussionThe overarching goal of the research team was to gather baseline clinical data, inspire further questioning, and inform future research. As a starting point, the primary aim of our overview survey was to collect demographic data regarding patients, and to assess the efficacy of treatment. We found patient demographics in the ARP clinics to be consistent with acupuncture clinics in other settings. 70% of ARP’s patients are women vs. 30% men, and 66% of patients’ chief complaints were musculoskeletal. This is comparable to numerous studies conducted in the United States. For example, the data collection program at the Oregon College of Oriental Medicine (OCOM)1 surveyed 2,485 patients and reported that 70% of patients were women, and 57.6% of patients presented with musculoskeletal issues as their chief complaint. OCOM utilized both the Measuring Your Medical Outcomes Profile (MYMOP)2 and Patient Reported Outcome Measurement Information System (PROMIS)3 as data collection instruments in a Practice Based Research (PBR) style setting, which is similar to the design utilized by the ARP. Chief complaints reported in the ARP clinics were also similar to those reported in US primary care clinics. In 2010, data were collected on 27,157 adults in a questionnaire done by the CDC utilizing the census bureau of the United States. Data showed that within three months of the survey, 17% of adults experienced a migraine or severe headache, 15% had experienced neck pain, 29% experienced low back pain, and 5% experienced face or jaw pain.4 In addition the CDC study reported musculoskeletal disorders, COPD, and digestive disorders as most prevalent. According to the CDC survey, of 229,505 adults, 118,972 had arthritic conditions or chronic joint issues. 20,974 had diabetes, and the third most prevalent disease was ulcers.4 This is not representative of treatments received or pursued, only prevalence of disease presentation. New DataAn unexpected outcome of the research was how the implementation of the survey helped practitioners hone their diagnostic skills. Analog pain scales, or any pain scales, do not work in the environment in Nepal. Pain scales are culturally limited. ARP’s patients have no context for scales of pain. They either have pain or they have no pain. Because we cannot utilize a pain scale that is key to interpreting patients’ pain, practitioners in Nepal have to change the way they gather their intake data and assess a patient’s condition. Practitioners are taught to utilize mostly information the patients provide to assess pain and prognosis. Because of the language barriers and context differences, patients in Nepal can only tell practitioners what their pain feels like in general terms (mild, moderate, or severe). Practitioners have to, based on their own objective data, determine extents of pain and to what extent that pain is interfering with a patient’s life, independence, and well-being. The actual implementation of the survey made practitioners take that step. With the survey in use, practitioners were able to more finitely assess where a patient was at the beginning and then assess progress throughout treatments. Often patients expect to regain fully what was lost and so the smaller steps of progress get lost. But when there are tangible, palpable changes, patients can see that they are making progress toward a goal. This keeps patients engaged in their own recovery as well as trusting in the medicine’s ability to help them achieve optimal health. BiasDoes the fact that this survey was conducted verbally by the treating practitioners create a greater capacity for bias? Most certainly this must be considered for a couple of reasons: the patients may feel pressured to give a positive response in order to continue receiving care or to receive optimum care, and the practitioners may lean toward the most positive outcomes when interpretation of a vague answer is needed. However, given the conditions and Nepal setting (predominant illiteracy, multiple languages, etc.), it was determined that this was the only responsible and logistical way to conduct this survey. Several factors that potentially reduce any bias must also be considered. For example, the large sample size and the fact that multiple practitioners and interpreters conducted the surveys. With a stronger emphasis on objective clinical findings, standardizing orthopedic testing was required when determining percentage of improvement or lack thereof. Further ResearchIn the future, the information gleaned from this survey may be used several ways. First of all, the practitioners, through the course of conducting this survey were enabled to successfully extract more specific data from the patient, both subjective and objective. This helped to better identify and quantify treatment progress and also lead clinicians through the process of formulating a treatment plan for each patient. This procedural part helped to facilitate discussions on how to evaluate pain and determine prognosis in this specific clinical setting. Because this was such a useful tool in the overall flow of the clinic, administrators are considering permanently implementing a similar process into the existing patient intake and follow-up protocol. Secondly, data from this survey will help the clinic plan for its supplies by identifying trends in patient care. Information that may have been useful to obtain, after evaluating this study, are the details about the 16% of patients that were referred to other practitioners for further evaluation and/or care. It would be helpful to track these patients and if possible to find out A) whether or not they went to where they were referred, and B) whether or not they returned to the ARP clinic for treatment. This is a potential area of future investigation. Knowing these details would further aid in serving this population in ways that would maximize resources. Based on the findings of this study ARP plans a future investigation into the use of mineral supplements and Chinese herbs in the treatment of the common complaint of persistent abdominal pain (gastritis). |
Table 1. Patient Gender |
|
Conclusion The data analysis will help ARP in documenting and legitimizing their clinic model. Low-cost, small-footprint facilities employing acupuncture as the primary treatment modality can deliver effective primary care in developing nations, rural environments, and underserved communities. References 1 Marx B, Rubin LH, Milley R, Hammerschlag R, Ackerman DL. A prospective patient-centered data collection program at an acupuncture and Oriental medicine teaching clinic. Journal of Alternative and Complementary Medicine, 2012 (in press). 2 Paterson C. Patient-centred outcome measurement. In Macpherson H. Hammerschlag R, Lewith G, Schnyer R. (eds) Acupuncture Research: Strategies for Establishing an Evidence Base. London. Churchill Livingstone, 2007. 3 Cella, D., Yount, S., Rothrock, N., Gershon, R., Cook, K., Reeve, B., Ader, D., & Fries, J. F., Bruce, B., Rose, M. (2007). The patient-reported outcomes measurement information system. Medical Care, 45(5), S3-S11. doi: 10.1097/01.mlr.0000258615.42478.55 4 Schiller JS, Lucas JW, Ward BW, Peregoy JA. Summary health statistics for U.S. adults: National Health Interview Survey, 2010. National Center for Health Statistics. Vital Health Stat 10(252). 2012. Other References Alreck, P. L., & Settle, R. B. (1995). The survey research handbook: Guidelines and strategies for conducting a survey. (2 ed.). Burr Ridge, IL: Irwin. Bausewein, C., Simon, S. T., Benalia, H., Downing, J., Mwangi-Powell, F. N., Daveson, B. A., Harding, R., & Higginson, I. J. (2011). Implementing patient reported outsome measures (proms) in palliative care- users’ cry for help. Health and Quality of Life Outcomes, 9(27), doi: 10.1186/1477-7525-9-27. Blue, C.M., Lopez, N. (2010). Towards Building the Oral Health Care Work Force: Who Are the New Dental Therapists? Journal of Dental Education, 75(1), 36-45. Castle, N. G., Brown, J., Hepner, K. A., & Hays, R. D. (2005). Review of the literature on survey instruments used to collect data on hospital patients’ perceptions of care. Health Services Research, 40(6), 1996-2017. doi: 10.1111/j.1475-6773.2005.00475.x. Epling, J.W., Morely, C.P., Ploutz-Snyder, R. (2011). Family physician attitudes in managing obesity: a cross-sectional survey study. Biomed Central Research Notes, 4(473), 1-8. Fowler, F. J. (1993). Survey research methods. (2 ed.). Newbury Park, CA: Sage. Meadows, K. A. (2011). Patient-reported outcome measures: An overview. British Journal of Community Nursing, 16(3), 146-151. Meadows, K. A. (2011). Patient-reported outcome measures: An overview. British Journal of Community Nursing, 16(3), 146-151. Mehrotra, A., Wang, M.C., Lave, J.R., Adams, J.L., McGlynn, E.A. (2008). Retail clinics, primary care physicians, and emergency departments: A comparison of patients’ visits. Health Affairs, 27(5), 1272-1282. doi: 10.1377/hlthaff.27.5.1272. Mold, J.W., Quattlebaum, C., Schinnerer, E., Boeckman, L., Orr, W., Hollabaugh, K. (2011). Identification by Primary Care Clinicians of Patients with Obstructive Sleep Apnea: A practice-based research network (PBRN) study. Journal of the American Board of Family Medicine, 24(2), 138-145. Sloane, P. D., Callahan, L., Kahwati, L., & Mitchell, M. (2006). Development of a practice-based patient cohort for primary care research. Family Medicine, 38(1), 50-58. Staniszewska, S., Haywood, K. L., Brett, J., & Tutton, L. (2012). Patient and public involvement in patient reported outcome measures: Evolution not revolution. Adis Online, 5(2), 79-87. doi: 1178-1653/12/0002-0079. |
|
News Blog
Latest News From Our Volunteers in Nepal
VOLUNTEER COMMUNITY CARE CLINICS IN NEPAL
Nepal remains one of the poorest countries in the world and has been plagued with political unrest and military conflict for the past decade. In 2015, a pair of major earthquakes devastated this small and fragile country.
Since 2008, the Acupuncture Relief Project has provided over 300,000 treatments to patients living in rural villages outside of Kathmandu Nepal. Our efforts include the treatment of patients living without access to modern medical care as well as people suffering from extreme poverty, substance abuse and social disfranchisement.
Common conditions include musculoskeletal pain, digestive pain, hypertension, diabetes, stroke rehabilitation, uterine prolapse, asthma, and recovery from tuberculosis treatment, typhoid fever, and surgery.
FEATURED CASE STUDIES
Rheumatoid Arthritis +

35-year-old female presents with multiple bilateral joint pain beginning 18 months previously and had received a diagnosis of…
Autism Spectrum Disorder +

20-year-old male patient presents with decreased mental capacity, which his mother states has been present since birth. He…
Spinal Trauma Sequelae with Osteoarthritis of Right Knee +
60-year-old female presents with spinal trauma sequela consisting of constant mid- to high grade pain and restricted flexion…
Chronic Vomiting +

80-year-old male presents with vomiting 20 minutes after each meal for 2 years. At the time of initial…
COMPASSION CONNECT : DOCUMENTARY SERIES

Episode 1
Rural Primary Care
In the aftermath of the 2015 Gorkha Earthquake, this episode explores the challenges of providing basic medical access for people living in rural areas.

Episode 2
Integrated Medicine
Acupuncture Relief Project tackles complicated medical cases through accurate assessment and the cooperation of both governmental and non-governmental agencies.

Episode 3
Working With The Government
Cooperation with the local government yields a unique opportunities to establish a new integrated medicine outpost in Bajra Barahi, Makawanpur, Nepal.

Episode 4
Case Management
Complicated medical cases require extraordinary effort. This episode follows 4-year-old Sushmita in her battle with tuberculosis.

Episode 5
Sober Recovery
Drug and alcohol abuse is a constant issue in both rural and urban areas of Nepal. Local customs and few treatment facilities prove difficult obstacles.

Episode 6
The Interpreters
Interpreters help make a critical connection between patients and practitioners. This episode explores the people that make our medicine possible and what it takes to do the job.

Episode 7
Future Doctors of Nepal
This episode looks at the people and the process of creating a new generation of Nepali rural health providers.

Compassion Connects
2012 Pilot Episode
In this 2011, documentary, Film-maker Tristan Stoch successfully illustrates many of the complexities of providing primary medical care in a third world environment.
From Our Blog
Research Paper
- Details
Our Mission
Acupuncture Relief Project, Inc. is a volunteer-based, 501(c)3 non-profit organization (Tax ID: 26-3335265). Our mission is to provide free medical support to those affected by poverty, conflict or disaster while offering an educationally meaningful experience to influence the professional development and personal growth of compassionate medical practitioners.