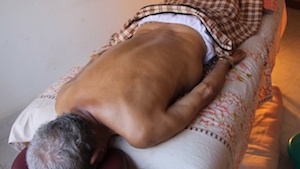
Rachael Haley BAppSci (TCM)
December 2014
OVERVIEW

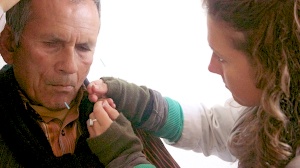
A 58-year-old man, of rural Nepal, presents with left hip pain, reduced strength and mobility in his left hip and significant muscle wasting in his left leg. After 30 electro-acupuncture treatments over 6 weeks and Traditional Chinese Medicine, the patient reports a significant decrease in his pain and inflammation levels and improved strength and muscle tone in his left leg.
Subjective
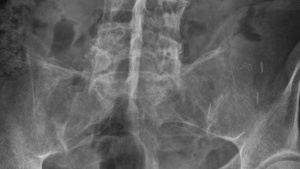
A 58-year-old male presents with chronic, left hip pain with intermittent referred pain into his lateral left leg; either down the iliotibial band (ITB) region or into the lateral lower leg. The hip pain is a throbbing, deep ache, worse in cold/damp weather and at night when he is trying to sleep. He is unable to straighten his left leg in bed due to pain and stiffness. The patient uses handmade wooden crutches to walk without fully weight-bearing on his left leg. He has been relying on these to walk for 6 years. The pain started over 6 years ago with a gradual onset without any history of trauma. The patient reported having an x-ray taken at this time, and repeated hospital visits for tests and prescriptions of western drugs over a 7 month period. After taking these medications (unknown) with minimal improvement, he threw out his medical reports and ceased treatment. After a prolonged period of rest, he was unable to weight-bear through his left leg without significant pain. He reports the x-ray described the joint as having a ‘jagged edge.’ Prior to the onset of his hip pain, the patient was an active farmer in rural Nepal.
Objective
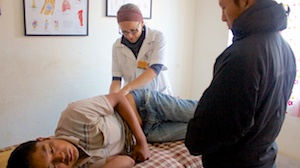
The patient presents with a slightly depressed demeanor. He is slight in build and stands with either all or most of his weight through his right leg. On observation, the patient’s left leg appears shorter, contracted at the hip and knee and has obvious muscle wasting in both the upper and lower leg. When walking to the clinic, he places minimal weight through his left leg, using the crutches as support. Due to postural imbalances, he cannot stand on both legs with equal weight distribution without left hip pain and his right knee having to flex about 30 degrees to get his left leg on the ground. The left iliac crest is visually higher than the right. The right ilium appears to be positioned more anteriorly. On his left hip, around his greater trochanter, there are 5 deep, large scars that are a result of abscesses that erupted after his initial onset of hip pain and hospital visits. The following orthopedic tests are conducted:
FABER’s test: Positive on left side
Straight leg raise: Negative on both sides
Thigh circumference is measured 15cm above the superior border of the patella to assess the extent of muscle wasting in his left thigh.
Right thigh measures 40cm.
Left thigh measures 35.5cm.
Palpation: A tight muscle band is palpated in the left erector spinae from T11 to L5, plus tightness in the left quadratus lumborum.
L1-S1 myotomes/muscle strength testing:L1-L3 (hip flexion/psoas) – unable to resist on the left side due to painL4-S2 (knee flexion/hamstrings) – 2 (Oxford scale)
|
Range-of-movement (ROM) |
Right |
Left |
|
Hip Passive Flexion (0-125°) |
125° |
80° with pain (a joint end feel cannot be felt) |
|
Hip Passive Internal Rotation (0-40° ) |
30° |
Minimal movement without pain |
|
Hip Passive External Rotation (0-45° ) |
30° |
Minimal movement without pain |
|
Knee active extension (0-15°) |
5° |
0° (shaky due to quadriceps weakness) |
Reflexes: Patellar and Achilles: Normal on both sides
Dermatomes: Lower limb sharp/dull test is normal apart from a small area on the left upper thigh (L1-L2 nerve distribution), which has reduced sharp sensation. Several deep, large abscess scars found around his left greater trochanter, possibly contributing to a slight sensory loss.
True leg length from ASIS to medial malleolus: Right 75cm, left 75cm
Apparent leg length from umbilicus to medial malleolus: Right 84cm, left 82cm
Postural imbalance may be causing apparent leg length discrepancy of 2cm, which is exaggerated by the contraction of his left knee and hip in a flexed position.
Extra note: On assessment of his crutches, 1 crutch is over an inch taller than the other and the handles are about 2 inches different in height. The patient is advised to trim down the taller crutch to make them the same height, and then the handle height can be adjusted if necessary.
Tongue: Swollen with a thick coat centrally
Pulse: Thin and tight
Assessment
DX: Osteoarthritis of the left hip (sequelae of osteoarticular tuberculosis)
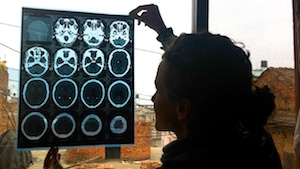
The patient’s reduced range-of-movement and the flexed position of the hip at rest, pain on weight-bearing and the description of a ‘jagged edge’ in his initial x-ray all indicate probable arthritic changes in the left hip. Initially, there was suspicion of infectious arthritis. However, considering the eruption of the abscesses several months after the initial onset of pain, it is unlikely that infectious arthritis was the initial cause of his pain. It is quite feasible to suspect that the patient may have had osteoarticular tuberculosis of the left hip. Osteoarticular tuberculosis is very rare in western countries. It is, however, still common in developing countries like Nepal. The hip joint is the second most common joint affected by the disease. Treatment of osteoarticular tuberculosis typically includes anti-microbial drug therapy of at least 9 months duration. This appears consistent with the patient reporting having taken a lot of western drugs and having several hospital appointments over the course of 7 months. This would also coincide with the abscess scars (they are a common complication of the disease). Other than anti-microbial therapy, an arthroplasty of the affected joint is often the solution if there is severe joint deformity. This currently is not accessible to the patient due to location, cost and health facilities in the region.
TCM DX: Wind-cold-damp bi syndrome
PROGNOSIS: Due to the fact that the condition has been left untreated for several years, it will take extensive treatment and continued care to maintain patient mobility and comfort levels. A complete cure is not expected.
Initial Plan
Acupuncture/electro-acupuncture treatment 5 days per week for 6 weeks
The focus is on local and distal points on the left hip and with electro-acupuncture to stimulate qi and blood flow, activate the muscles and reduce inflammation in the joint. As pain levels decrease, encouragement to place more weight through the left leg will be advised. Adjunct modalities when time permits include myofascial release/cupping to address muscle imbalances and increase circulation. Exercises will be prescribed to help build muscles in the left quadriceps, which will help support the hip joint. Chinese herbal medicine will be prescribed to improve patient energy levels and decrease pain and inflammation. Patient education regarding his expectations of improvement and self-care at home will be prescribed.
Typical treatment:
Supine/right lateral recumbent: ST36, SP10, GB34, LV3, LI4, SP6, SI3, BL62, 5 local Ah Shi points of the left hip and local needling around the scar tissue near the left greater trochanter
Electro-stimulation (2 pairs) - left gluteus medius, vastus medialis origin (SP10) and left tibialis anterior (ST36), peroneal muscle (GB34); 2/100 hertz
Alternate treatment:
Seated forward: Hwa Tou Jia Ji points, particularly on the left lumbar spine (deep paraspinals), to release the taught band of muscle
Additions to treatment (time permitting):
Cupping: Left lumbar spine and right thoracic; Left hip and ITB
Muscle release: Psoas/tensor fasciae latae (TFL)/adductors
Exercises: Isometric contraction of the left quadriceps muscles to activate and assess muscle tone
Herbal formula: Du Huo Ji Shang Wan
Outcome
After 6 weeks of treatment, the patient reported occasional dull pain in the left calf and thigh. Some nights, he was able to sleep pain-free. He experienced aching only in cold weather or after sitting for long periods of time. Sharp/dull dermatome testing became equal on left and right in L1-L2 nerve distribution. Range-of-movement testing showed a great improvement in passive, left hip flexion to 90 degrees without pain. The joint had a solid end feel at this range with application of overpressure. Knee flexion and extension strength became equal on both sides without pain (Oxford scale - 5). He attained 10° of internal rotation and 15° of external rotation in his left hip without pain. Apparent leg length remained the same and left thigh circumference, measuring muscle tone, increased by ½cm.
Continued Plan
It is recommended the patient continue with treatment for as long as it is available to him.
Even though these modalities appear to decrease pain and inflammation, it is possible the patient would see further improvement with a modality that specializes in postural rebalancing, exercise and reeducation. Without further imaging, it is hard to give an accurate prognosis. It is likely, in a western culture, with more resources and affordability, this case would have been treated with a left hip arthroplasty and follow up rehabilitation care.
Discussion
Due to the severity and chronic nature of the patient’s condition, a full resolution of his pain was not expected. The history of onset and initial diagnosis are still unclear. The environment in rural Nepal creates the challenge of walking up and down rocky paths, which makes walking for the patient more difficult. Doing this on crutches that were uneven in height likely contributed to the patient’s postural imbalance, particularly the taught band of muscle in his left lumbar region. Because of the chronic nature of the patient’s condition, it was imperative to discuss with him the need for continued care and management of his pain and mobility. The Chinese herbal formula, Du Huo Ji Sheng Wan, has been shown to inhibit inflammatory responses and pain in some biomedical studies on animals. It may also increase blood circulation and enhance the function of macrophages to clear inflammatory tissues. It is likely this contributed to the patient’s progress by decreasing inflammation and increasing circulation in the joint.