Joey Chan BHkin Dip AOMj RAc
February 2013
OVERVIEW
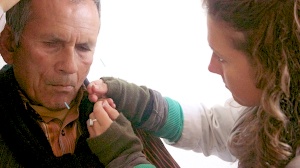
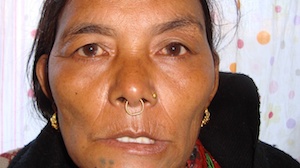 A 50-year-old female with Bell’s palsy presents with hemi-facial paralysis involving the eye and the mouth. After 5 weeks, 10 acupuncture treatments and 2 months of Chinese herbal medicine, she experienced a 90% recovery.
A 50-year-old female with Bell’s palsy presents with hemi-facial paralysis involving the eye and the mouth. After 5 weeks, 10 acupuncture treatments and 2 months of Chinese herbal medicine, she experienced a 90% recovery.
Subjective
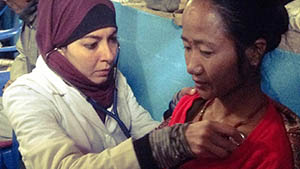
Patient is a 50-year-old female presenting with right side paralysis of the face involving the forehead, eyes and mouth. The paralysis developed suddenly, 1 week prior to her first consultation at the clinic. Patient recalls having a low fever and chills for 3 days, with a slight sore throat and cough. On the 4th day, she woke with hemi-facial paralysis marked by an inability to close her right eye, with additional tearing and swelling of the right eye. She reports she has not slept at all for 7 days because her affected eye will not close. Patient describes symptoms of forehead pain and tightness, which can lead to twitching of the eye during severe pain. She also reports eye twitching when she is in a cold environment.
She experiences constant vertex and occipital headache, described as deep and moving pain, in addition to sharp pain behind the right ear. The left side of her mouth is being pulled and is tight, while the right side of the mouth is painful. She describes her face as being numb and drying up. She also feels chills and dizziness, usually in the morning and evening. She states that her overall body temperature alternates between hot and cold, though her hands and feet always feel cold. She reports her energy is very low, her body feels heavy, and she has no appetite. She is losing her sense of taste. She states that there has been no improvements since the incident and she has not seen any other health care providers.
OBJECTIVE
Patient appears to be weak and has low energy. She is thin with her cheekbones protruding. She talks in a quiet and slow voice. She looks tired and her eyes are always looking down. The right side of her face is expressionless and the left side is tight. The patient’s right eyelid droops down covering ¼ of her eye. The patient’s right eyebrow and
eye is asymmetrical to the left, with the right side sitting ¼ inch lower than the left side.
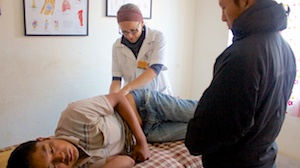
Facial expression tests of the seventh cranial nerve consist of blinking the eyes, closing the eyes, wrinkling the forehead, smiling and frowning. When tested, patient is unable to close her left eye or blink. She can only close the eye ¼ of the way. The patient’s right forehead does not wrinkle when compared to the left side. The patient refuses
to smile and frown when asked. Sharp/dull sensory test shows lack of differentiation on the right side of the face. Motor facial tests of saying the sound “E” and “O” show asymmetry of the mouth. Saying “A” is symmetrical.
Patient’s demeanour appears low and her eyes dull. Her face color is dark and dull and her nails are pale. Her tongue is dry with a red heart tip, white coat and a quiver. Her pulse is deep and weak and very faint on the right.
ASSESSMENT
DX: Asymmetrical facial expressions of the right side of the forehead, eyebrows, eye and mouth and the loss of taste shows that the seventh cranial nerve is affected, leading to the diagnosis of Bell’s palsy. Damage to the orbicular oculi is shown from the lack of passive eyelid movement. Occipitalis and frontalis muscles responsible for lifting
the eyebrows and wrinkling the forehead are also affected. Mentalis, risorius, levator labii superioris and depressor labii inferioris damage is seen from the asymmetrical facial expressions of saying E, O and smiling.
Damage of the seventh cranial nerve affects the taste sensory of the anterior 2/3 of the tongue.
TCM DX: External wind-cold attack of the Bladder Taiyang channel leading to blockage in the Bladder Taiyang and Stomach Yangming channels, with underlying qi and blood deficiency and dampness from Spleen qi deficiency.
The patient’s symptoms began with a wind-cold attack, presenting with fever and chills, slight sore throat and cough. The wind-cold entered the Bladder and Stomach channels of the face, leading to wind invasion and blockage of these channels. Wind-cold symptoms shown are vertex and occipital headache around BL10, pain at SJ17 on
the right side, twitching of the eye that is worse in a cold environment, and a quivering tongue. Blockage along the Stomach and Bladder channels on the face is shown by hemi-facial paralysis and lack of sensation on the face.
Qi and blood deficiency signs and symptoms are fatigue, poor appetite, dull eyes, dull and dark facial complexion, pale nails, numbness of the face, dry tongue and a deep weak and faint pulse.
Dampness signs are shown on the tongue with a white coating, as well as a heavy feeling in the body.
PROGNOSIS: Patient seeks treatment at this clinic 1 week after onset of initial symptoms. Improvement is more likely due to early diagnosis and treatment. Significant improvement may be possible with a course of 10 acupuncture treatments and 2 months of Chinese herbal medicine.
PLAN
Treatment principle: First expel wind-cold and then tonify Spleen qi and blood and resolve damp.
Treatment: Acupuncture 2-3 times per week for 10 treatments before re-evaluating; Herbal treatment for 2 months.
Treatment approach is to expel wind-cold in the Bladder Taiyang channel, treat locally on the face to unblock channels, tonify qi and blood and resolve damp.
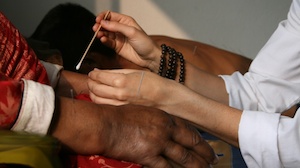
Typical treatment: BL2, BL10, GB8, ST4, ST5, ST6, DU14, DU20, SJ17, Yu Yao, SP6, ST36, LI4. Other points included are ST40, SJ5, SI19, SJ23, DU16, GB2. A technique of pulling the drooping eyelid up prior to needling is used. Local eye and mouth points are used on the right side. Electro-acupuncture is used on the face from the eighth treatment onwards when she had more qi and blood to support stronger stimulation. The electro-acupuncture setting is 100/2 hertz with mixed macro amp for 20 minutes. Typical electro-acupuncture points connect SJ17 to DU16 and ST3 to ST5.
Jing Fang Bai Du San and Chuan Xiong Wan are given for 2 weeks to expel wind-cold. Jing Fang Bai Du San tablets are given for 3 days, TID. Then Chuan Xiong Wan tablets are given for 11 days, TID.
The formula is then switched to Gui Pi Wan for 2 weeks to tonfiy qi and blood. Xiang Sha Liu Jun Zi Tang is given for a week, afterwards, to tonify Spleen qi and move damp. 3 weeks of Yu Ping Feng San is given after the last acupuncture treatment to tonify wei qi.
Patient is advised to eat more meat, egg or alternative protein in order to increase her energy, qi and blood. Patient is also advised to do facial exercises of saying “A, E and O.”
OUTCOME
At the fourth consultation, the patient reported that there was no more pain in her forehead, with only an occipital headache. Her sense of taste returned. She reported not feeling the needles on the right side of her face during the initial treatment, but could now feel the needles.
Her demeanour and energy appeared much better. Her eyelid drooped down to cover 1/8 of her eye and she was able to close her right eye ¾ of the way. She was finally willing to show her smile. It was asymmetrical. The right side of her mouth was still expressionless and the left side tight. The patient could now differentiate between sharp/dull sensations on the affected side. The patient’s tongue had a red tip, thick white coat and no tremor.
From treatment-to-treatment, there was considerable improvement. There were visible improvements of the eye and mouth. With each visit, she had more strength in her voice, and color in her face.
On the eighth treatment, she asked if she could discontinue treatment since she felt 80% better. Her eye and forehead had the most significant improvements, though the patient’s mouth was still asymmetrical. Her pulse was weak, but stronger than before.
She was advised to come for the full 10 treatment since she was not fully recovered. At the tenth treatment, all tests were performed and an improvement was shown in all the tests. The patient could close her eyes fully and blink properly. Facial expressions of raising the eyebrows were symmetrical. Sharp/dull sensory tests showed the same sensations on both sides. Motor facial tests of saying the sound “E” and “O” showed slight asymmetry of the mouth. Patient reported a good appetite. She was sleeping 9 hours per night without interruption, she had more energy and her body felt lighter. There was slight pain behind the right ear and the left side of the mouth was slightly tight.
After 10 acupuncture treatments, she was not able to come anymore. Therefore, 3 weeks of Yu Ping Feng San was prescribed.
CONCLUSION
This patient showed rapid improvement from acupuncture and herbal medicine for Bell’s palsy. She showed a significant improvement from acute Bell’s palsy with herbal medicine and 10 acupuncture treatments 2- 3 times per week for 5 weeks. The patient was given 3 weeks of herbal medicine to boost her immune system after her 10th
acupuncture treatment. For this patient, 20 acupuncture treatments would be a more appropriate course of treatment. 90% recovery was shown with 10 treatments. If recovery is to follow the same course, full recovery may be possible at 15 acupuncture treatments; and 5 more treatments after to strengthen her immune system. This case demonstrates that with early diagnosis, and continuous and frequent treatment of acute Bell’s palsy using acupuncture and Chinese herbal medicine, significant results are highly possible.
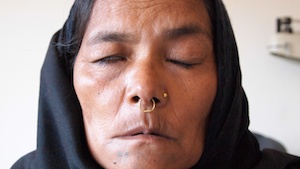
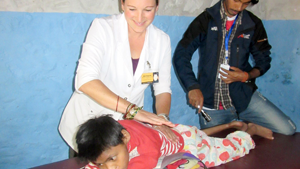
3rd visit - eye closed half way

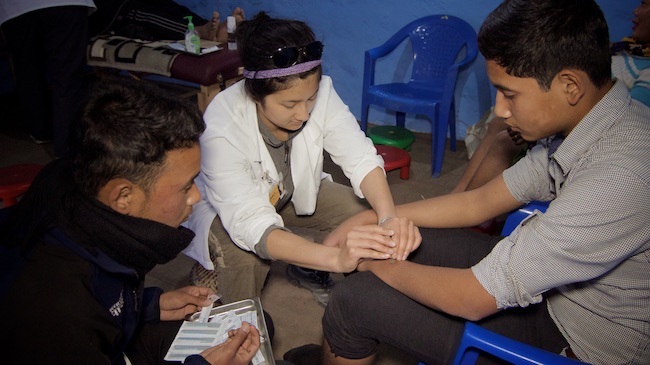
6th treatment - saying the sound “E”
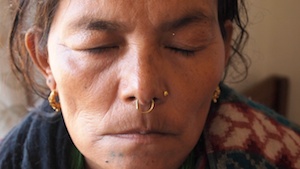
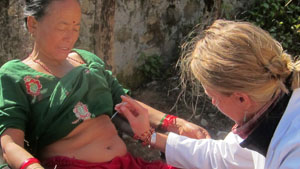
8th treatment - eye closed with no gap
More color in face, more energy, gained weight

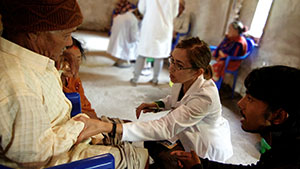
10th treatment- saying the sound “E”