When it's all said and done, leading a team in any capacity is not an easy job. Being a medical volunteer here also stretches each of us. I thank my team for working from day one in a new remote town, and also a new clinic! Yes, newness can bring challenges, but, like any spiritual growth, there is major relief that comes only pushing through the most climactic and painful time. It's like sitting down to meditate and you are faced with all the itches and discomforts in your body. You want to jump up and scream and run from it, but you know, only sitting a few moments longer will bring the most blissful freedom you can imagine.
How do I show up every day to lead others through their tunnel to the light? How can I be a true leader when I'm still the student; still learning how to surrender myself? How to let go of my own ego, time and time again, in the face of challenges? How to catch myself when I speak incorrectly of others? And how to guide with patients and love and right action? This is no easy task. Others who come to lead a team may not have taken this task this way, as there is so much “medical work to do”, but I did. And I have so much to still learn. No expectations. Practicing constant gratitude to The Most High. Letting go. Letting Qi flow. These are some of the big lessons. Maybe of a lifetime.

In the Compassion Connects video by ARP, Andrew Schlabach tells his team that one of most difficult things of this work, is that one case you return home thinking about. That one patient you couldn't help just right. “You forget about the hundreds of patients you helped and they got better, but it's that one patient that stays with you.” This has happened to me. And I can't stop thinking about her.
In case review one afternoon, practitioner Shin Kim introduced us to a 23 year old female who was coming in for back and neck pain.
She had a large plastic bag filled with x-rays, medical charts from various clinics and hospitals, lab tests, and a stack of medical bills. Also seen in her charts, was a referral letter with a detailed clinical summary, written by the awesome volunteer practitioner Bex Groebner from Camp C, February 2015.
It stated:
“…We are concerned about the potential of spinal tuberculosis (TB) for Ms. R.S. symptoms. We would like to rule this out before moving on to more complex diagnoses.”
The patient had a Positive Mantoux (TB) test from the health-post in Bimphedi. She also had spinal X-ray, MRI and CT scan, showing a lesion at the 12th thoracic vertebra, high white blood cells and inflammation markers, as well as low hemoglobin.
The illness began 18 months before her visit with Bex, when she presented with:
High fever, chills, headaches, nausea and vomiting, loss of consciousness, daily vertigo, photophobia, insomnia, tender mid abdomen and flank, and high level of pain upon palpation to neck and back. She was treated with high doses of antibiotics then, and since that time was still experiencing most of these symptoms.*
This patient R.S. was referred to get a proper diagnosis and care over 9 months ago, but here she is showing back up at our clinic in Bimphedi! Shin explained how she expressed concern because she still had not gotten any diagnosis besides “Anemia and Spinal Degeneration”, and furthermore no relief of her back pain and symptoms. She reported being more than upset that she has been sent from one place to another for months, spending so much money, and that she was in great despair. Shin also stated that she looked skinny and weak, with dark circles under her eyes, and that her back muscles were super tight. He gave her an acupuncture treatment of mostly back points that she could hardly tolerate due to pain, and started her on Chinese Herbs.

I went in to see her the next visit myself to better understand her situation, and try and come to a quick and decisive plan of action.
From the moment I sat down she started talking about all her complaints, confirming that everything she had reported back in Winter of 2015, she was still experiencing. The only thing that was better was that she was a little less nauseous after the few days of herbs, and was vomiting less after meals. She was very emotional, both sad with tears and also angry.
She was very uncomfortable laying on her back and could not handle minor pressure when I tried to massage her in this position, nor settle long enough for a craniosacral treatment. She demanded to be treated sitting in the massage chair.
I talked with her about my concern that she had a positive Mantoux test and that, just like Bex had requested, it was important that she ruled out Spinal TB. She told me “I wanted to have a biopsy to my spine as well, but the doctor I saw said I didn't need one, and wouldn't let me get one”. Instead she just kept getting referred for more x-rays and labs. I told her that this has been a recurring issue we have seen with other patients. Unfortunately it is very hard to get the proper doctors in Nepal to do TB testing, diagnose it correctly, and then get the proper antibiotics administered by the WHO. This is why I felt strongly she should try again to go get the biopsy.
This was my concern and why she remained on my mind - How many patients are there in this world who are not receiving proper medical follow-up and care? If the patient doesn't have support, especially if they are illiterate, poor, elderly, have mental health issues, or simply fear medical establishments, do they ever receive the medical care they truly need? Even in America, who is responsible for the patient once they are discharged? Once they are referred on? Sent home with a handful of medications?
ARP does its best to teach and instill in the volunteers to have proper discussion, explanation and agreements with patients of what is expected, and to have clear follow up. However, the doctors we refer our patients to do not always send the patients back to us. Over the last year we have started to write this in the referral letters, and communicate to the patients the need to return to us. Somehow between the camps this patient got lost. Perhaps this was due to the earthquake coinciding with that period of time. But I also think this was because she didn't end up being administered in the hospital she was first sent to. You hope that once she makes it there she would be taken care of and treated, but instead she was sent in circles again, from one doctor to another. The general population put so much trust into the medical professionals that they don't question, or rather, even know what to question, to get the answers they need for adequate help!
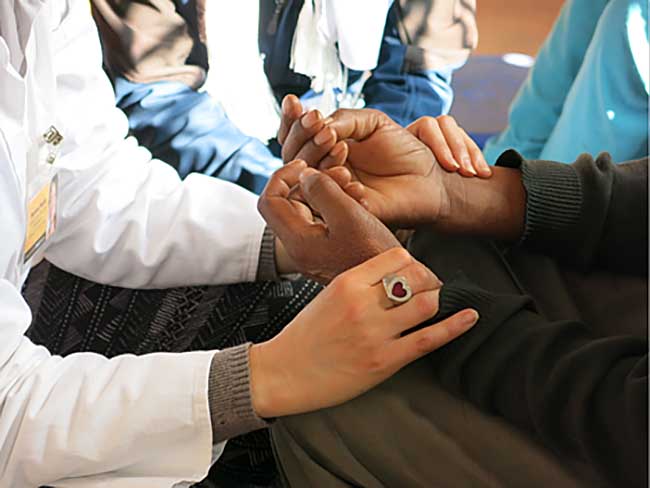
After sending her back to the TB hospital in Kathmandu, Andrew and Tsering went to visit her after the surgery. They listened to her and comforted her, which I believe is the most therapeutic offering ever, as “people truly start to heal the moment they feel heard”. Tsering told me that just that act of listening, he saw a shift in her energy and demeanor. Our relationship to pain and the power of emotions is an interesting thing we know through science, and through Chinese Medicine. Andrew spent a lot of time counseling her upon not doing any more x-rays for now, since she did more than enough already, and that she needs this time mostly to rest. He also taught her some stretches for her back and chest. He then asked her if she was willing to stay in her hometown of Kathmandu in the future, and receive acupuncture, body work, and herbs from a local clinic for minimal fee, which she agreed to. Tsering then let her know we would follow up with her in a few days once she had the biopsy results.
As for the biopsy results, they were negative for TB. I believe this result and having an answer was a relief for her.
However, I still can't help but wonder, why is she so sick? After being sent around to so many doctors, she still doesn't have an allopathic diagnosis besides “Spinal Degeneration”. How many patients show up in our office with this same story? If you have done the testing they are able to do, and get an answer of “what it is not, at this time”, is that enough?

The first thing I think about was the possibility of the positive Mantaux TB test being wrong. We know that False-Positive reactions can happen.
Then I think, perhaps we are just looking at someone with pain from osteopathy and compression, as the MRI’s show, due to years of carrying heavy loads. Perhaps she has emotional and mental pain from a history I know nothing about. Maybe she is so anxious from going to one doctor to another looking for answers, spending so much money and energy. With more time with her, more listening, perhaps I would have clarity about her distress and illness.
I also consider what else it could be from an allopathic perspective, and come to the realization that even with getting a diagnosis for some pretty severe diseases, we would still be administering symptom control to improve her quality of life. This would mostly be pain relief treatments. In the allopathic medical system she would probably be given a lifetime use of pharmaceuticals, such as strong anti-inflammatory drugs, that she may not be able to fund. Working to help maintain mobility and control spasticity through stretching and exercise, would also be important, as would receiving micronutrients, promoting organ function and hormonal balance, and treating other accompanying symptoms including appetite, bowel health, insomnia, and definitely emotional trauma and stress management. After thinking about it, she would be getting this long term supportive care and treatments from the local Acupuncturist we connected her to. This is the power of Chinese Medicine system, we look at patterns of disease our patients presents with and treat accordingly. Although our diagnosis has a different name, often, even when the allopathic diagnosis isn’t known or understood, we can still greatly help by this approach.

Tsering told me upon that second visit in Kathmandu, she was in better spirits, and reported she was feeling much better with the herbs. She had actually sent her relative in Bimphedi to us, to get more herbs for her while she was in the hospital. So yes, there was progress and help here.
What I think about most now is how fortunate we have someone like Tsering on the team, to not only connect her to the right people, but actually cares enough about each patient to take the time and energy to assist us with their case! This is very rare in a NGO relief-work organization, and has highlighted the importance of having someone for this role for these patients to not be left to the way-side. She is not the only patient ARP has had to follow up on in this way, and won't be the last. We see patients everyday who need more advanced medical treatments than what we can offer, most of which are in Kathmandu. Not everyone however has the ability to receive it, but the handful who do, we still consider "our" patients. This is what it means to give patientcare, and not just patient treatment.

In Nepal I can let go of living conditions and any attached expectations of the way of life, because that is how it is when you travel. Let go of hot water, choice of food. Let go of being comfortable, of having consistent transportation. You become one with the people, and the place.
But how can you let go of fighting for a persons health, and humanitarian efforts? When you know it shouldn't be this way. That it doesn't have to be.
It is a balance between doing everything in your ability, and then trusting that the rest is up to a Higher Power. And still it breaks your heart. But I guess, like I have said many times this last year, it is that breaking of my heart that causes it to open.
And maybe that is what it takes to keep us on this path of service, of returning year after year. Not many people understand it. I have come back to that same poem I wrote in my last ARP blog (http://www.acupuncturereliefproject.org/news-blog/202-meant-to-be-together) in 2013, the lessons of just Being. Of surrendering. Of knowing that this life is a constant flux.
“Your hand opens and closes
and opens and closes.
If it were always a fist or always stretched open,
you would be paralyzed.
Your deepest presence is in every small
contracting
and expanding,
The two as beautifully balanced and coordinated
as bird-wings.” (Rumi)

At the end of it all I see clearly that we medical volunteers return home, but the work continues for the interpreters, ARP board members, and especially for Tsering, Satyamohan, and Andrew who show up to work daily, or return year after year, giving everything they have to these patients in need. This is not an easy task by any means, trust me, and it takes a "one of a kind" spirit.
Like Prophet Mohammad (p.b.u.h.) said, "The leader of a people is their servant."
I know it isn't much, but I want to take the time to thank them, and wish them all the best to keep moving forward in the years to come (God willing).
Asiya Mahdiyah Shoot MS. LAc. EAMP, LMP, CNP, CD(DONA)
*For more information please look out for her case study.











